New Drug Proves Helpful for Treating Long-Term Insomnia

Researchers at Duke University Medical Center and elsewhere have completed the first large-scale study demonstrating sustained efficacy of a medication to treat insomnia for a period of six months.
Eszopiclone (trade name Estorra), was administered nightly to patients with chronic insomnia and led to significant improvement in patients’ ability to fall asleep and stay asleep and in the quality of their sleep without any evidence of a loss of effect over time, the researchers said. Prior to this study, the longest large-scale, placebo-controlled study of a sleep medication for insomnia lasted five weeks.
The data further demonstrate that improvements in sleep were associated with consistent improvements in the patients’ ratings of their capacity to function well during the day, said the researchers. Impairments in daytime function are one aspect of chronic insomnia, and the new study represents the first time any sleep medication has been shown to consistently improve all of the components that define insomnia, they said.
Insomnia is the perception of inadequate or poor-quality sleep that is accompanied by significant distress or impaired function. It is considered to be chronic if it occurs on most nights and lasts a month or more, according to the National Institute of Health.
“I believe that this study is a milestone for research into insomnia treatments,” said Andrew Krystal, M.D., lead study author and associate professor of psychiatry and director of the Sleep Research Laboratory and Insomnia Clinic at Duke. “It greatly extends the period of time that a medication has been definitively shown to help people suffering from insomnia and it establishes that studies of longer-term drug treatment of insomnia are not only feasible but can be safely performed.”
The research findings appear in the Nov. 1, 2003, issue of the journal Sleep.
The researchers randomized 788 patients aged 21 to 69 into a six-month, double-blind, placebo-controlled study of three-milligram nightly doses of eszopiclone to treat their insomnia. Participants were required to meet the standard criteria used to make the clinical diagnosis of primary insomnia and to report, on average, less than six-and-a-half hours of sleep per night, or that it took at least 30 minutes to fall asleep for at least one month prior to being screened for the study.
According to Krystal, the results provide the first step toward establishing an empirical base to guide the long-term treatment of chronic insomnia with medication. The findings suggest that eszopiclone has the potential to provide doctors with a treatment option that could be prescribed for patients who require longer-term treatment. The data demonstrate that eszopiclone is safe and could be helpful. By opening the door for future studies of longer-term treatments for insomnia, this study represents an important step in the evolution toward improving treatment options for patients with chronic insomnia, he added.
“The fact that eszopiclone improved not only the difficulties in sleep that patients experience but also their reports of problems they typically experience during their waking hours, suggests the need for a change in our perspective,” Krystal said. “The idea that effective treatment should address the entire spectrum of difficulties experienced by patients with insomnia is really a new way of thinking for the field.”
An estimated 2.5 percent of Americans take sleep medications for insomnia in any given year, the researchers report. Of these, about 23 percent take such medications on a nightly basis for four months or longer. However, clinical research studies have examined the use of such drugs for an average use of one week. The problem with this, the researchers say, is that long-term drug treatment is being carried out without the existence of research supporting that long-term use is safe or effective in adults.
Nearly 60 percent of American adults surveyed about their sleep habits say they experience sleep problems more than a few times each week, according to the National Sleep Foundation. In their 2003 “Sleep in America” poll, the group found that insomnia is the most common sleep problem and that only one in eight older adults say their problems have been diagnosed.
Of the many people who report sleep problems, 20 to 36 percent report that their problem lasted for more than one year. Thus, the researchers say, it is not surprising that so many people are using sleep medications for long periods of time.
Research funding was supported by Sepracor, Inc., the manufacturer of eszopiclone, a compound currently under review by the Food and Drug Administration.
Krystal has previously designed and conducted other studies for Sepracor and has served on an advisory board there.
Other authors on the study include James Walsh, Ph.D., of St. John’s/St. Luke’s Hospital and St. Louis University; Eugene Laska, Ph.D., of Nathan Klein Institute for Psychiatric Research and New York University School of Medicine; Judy Caron, Ph.D., of Sepracor, Inc. in Marlborough, Mass.; and David Amato, Ph.D., Thomas Wessel, Ph.D., and Thomas Roth, Ph.D., all of Henry Ford Sleep Disorders Center in Detroit, Mich.
Media Contact
More Information:
http://dukemednews.org/news/article.php?id=7126All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Targeted use of enfortumab vedotin for the treatment of advanced urothelial carcinoma
New study identifies NECTIN4 amplification as a promising biomarker – Under the leadership of PD Dr. Niklas Klümper, Assistant Physician at the Department of Urology at the University Hospital Bonn…
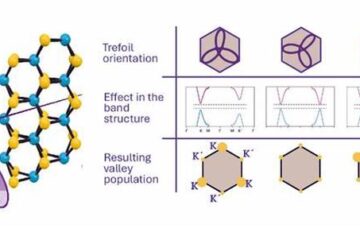
A novel universal light-based technique
…to control valley polarization in bulk materials. An international team of researchers reports in Nature a new method that achieves valley polarization in centrosymmetric bulk materials in a non-material-specific way…

How evolution has optimised the magnetic sensor in birds
The magnetic sense of migratory birds is probably based on the protein cryptochrome 4, and a genetic study has now provided further support for this theory. A team of researchers…





















