Brain function in schizophrenia can improve with support, holds promise for cognitive rehabilitation

Need cues, memory aids
When encouraged to use memorization strategies commonly employed by healthy individuals, people with schizophrenia can be helped to remember information just as well as their healthy counterparts, a process that in itself seems to spur a normalization of memory-related activities in the brains of people with schizophrenia, suggests new research from Washington University in St. Louis.
Memory study shows brain function in schizophrenia can improve with support, holds promise for cognitive rehabilitation
For decades, schizophrenia treatment has relied on powerful drugs to control the disease’s most debilitating symptoms — hallucinations, delusions and paranoia – often ignoring seemingly less ominous problems associated with learning, memory, attention and other cognitive functions that are so basic to everyday life.
Now, as part of a new wave of research aimed at helping people with schizophrenia lead fuller, more normal lives, a study at Washington University in St. Louis has demonstrated that people with schizophrenia can be helped to remember things just as well as healthy subjects as long as they are given proper cues and memory aids.
The study suggests a new way of understanding the cognitive problems that underlie schizophrenia, and offers hope that schizophrenia’s suffering can be alleviated through the development of more effective cognitive rehabilitation programs.
“These are interesting findings for a number of reasons,” said Aaron Bonner-Jackson, lead author of the study and psychology doctoral student in Arts & Sciences at Washington University.
“First, they demonstrate that individuals with schizophrenia possess the ability to learn to the same degree as healthy control subjects, although they may not spontaneously use such memory strategies in everyday life.
“Second, our findings also indicate that use of these beneficial strategies can actually cause memory-related brain activity in schizophrenia to ’look like’ brain activity in healthy controls. Thus, there seems to be a strong tie between the strategies used to remember words and the brain activity that results when people try to remember information.”
How to reduce, eliminate memory problems
Researchers have long recognized that schizophrenia is associated with a wide range of memory problems, but only recently have studies focused on determining whether these memory problems could be somehow reduced or eliminated.
The Washington University study, published in the July 1 issue of the journal Biological Psychiatry, confirms that memory problems in schizophrenia can indeed be reduced and suggests that helping people use the right memorization strategy is critical to success.
“Typically, when people are encouraged to process words more “deeply,” they will be more likely to remember those words later, as opposed to words that they process “shallowly,” which they are less likely to remember,” Bonner-Jackson said.
“This is what we found in our schizophrenia group: when we required them to process words in a deep, semantic manner, they remembered significantly more words than when they processed words in a shallow manner.”
The use of more effective memory strategies not only improves recall, it also seems to trigger a more normal pattern of memory-related brain activities.
“In addition to showing improved memory for words that they had processed deeply, the schizophrenia group also activated a number of brain regions that have been shown to be crucial for verbal processing and memory function in healthy control subjects,” Bonner-Jackson said.
“For the most part, these brain regions had been shown to be less active in schizophrenia during memory tasks. The results of our study would suggest that these regions were not found to be active because the participants with schizophrenia were most likely not engaging in advantageous memory strategies.”
While the use of “deep” semantic memory processing seems to help most people with schizophrenia focus memory tasks in areas of the brain normally used for this purpose, the study found that some of the poorest performing patients continued to activate brain areas outside this optimal zone. This additional activation does not seem compensatory in the sense of helping or supporting memory functions, rather it may simply serve as a neural marker of who is having the most difficulty, researchers suggest.
In addition to Bonner-Jackson, the study’s co-authors are John Csernansky, M.D., the Gregory B. Couch Professor of Psychiatry in the School of Medicine; Deanna Barch, Ph.D., associate professor of psychology in Arts & Sciences and assistant professor of psychiatry and radiology in the School of Medicine; and Kristen Haut, then a research assistant in psychology in Arts & Sciences; all of Washington University.
Good news for cognitive rehab techniques
The team’s findings are positive news for those now pursuing cognitive rehabilitation techniques for schizophrenia, Barch said.
“Our results suggest that poor memory function in schizophrenia is in part due to changes in the use of strategies, and does not reflect an immutable inability to learn new information,” Barch said. “Individuals with schizophrenia can benefit, as much as healthy individuals, from external support for the use of effective memory strategies. In fact, with support, the performance of people with schizophrenia is much more similar to that of healthy individuals than in situations where people have to generate their own memorization strategies.”
The study was supported through several grants from the National Institute of Mental Health, including a grant to the Silvio O. Conte Center for the Neuroscience of Mental Disorders in the School of Medicine at Washington University in St. Louis.
“Developing treatments for the cognitive problems associated with schizophrenia is one of our highest priorities, since these problems are present very early in the illness and even occur in the relatives of patients with schizophrenia. Thus, they may be closely related to the genetic underpinnings of the disorder,” said Csernansky, director of the Conte Center.
The Conte Center is now looking for more people to take part in its studies, including healthy people, but especially people with schizophrenia and their siblings. For more information, visit the center’s Web site (http://conte.wustl.edu) or call: 314-747-2160.
Media Contact
More Information:
http://www.wustl.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
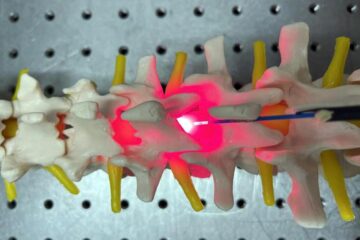
Red light therapy for repairing spinal cord injury passes milestone
Patients with spinal cord injury (SCI) could benefit from a future treatment to repair nerve connections using red and near-infrared light. The method, invented by scientists at the University of…

Insect research is revolutionized by technology
New technologies can revolutionise insect research and environmental monitoring. By using DNA, images, sounds and flight patterns analysed by AI, it’s possible to gain new insights into the world of…

X-ray satellite XMM-newton sees ‘space clover’ in a new light
Astronomers have discovered enormous circular radio features of unknown origin around some galaxies. Now, new observations of one dubbed the Cloverleaf suggest it was created by clashing groups of galaxies….





















