Common diabetes drug causes arteries to spasm, endangering heart

The oral medications most widely used to lower blood-sugar levels in patients with type 2 diabetes are likely to increase the risk of spasm of the coronary arteries, reports a University of Chicago-based research team in the July 15 issue of the Journal of Clinical Investigation. Constricted arteries increase blood pressure and decrease blood flow to the heart, causing chest pain and even sudden death, shows the study, which focused on mice with a genetic defect that duplicates the actions of these drugs.
Sulfonylurea drugs are the mainstay of therapy for non-insulin-dependent diabetes, which affects an estimated 15 million people in the United States. These drugs stimulate the beta cells of the pancreas to squeeze out more insulin and also make insulin more effective.
Since the early 1970s, however, several studies have suggested that sulfonylurea drugs may actually increase cardiovascular problems in diabetic patients. The link between these drugs and heart damage has been disputed, because it was not clear — until now — exactly how such medications increased cardiovascular risk. The new study demonstrates a direct link between the receptor for sulfonylurea drugs and coronary arterial spasm, heart damage and death.
“This study, even though it involved mice, argues that from now on we should think twice, or maybe more than twice, about using the sulfonylureas, particularly if other options are available,” said Elizabeth McNally, M.D., Ph.D., a cardiologist at the University of Chicago and director of the study. She adds that “other options are always available.”
The discovery grew out of a laboratory problem. In 1999, William Chutkow, an M.D.-Ph.D. student working in the lab of diabetes specialist Charles Burant at the University of Chicago (Burant is now at U. Michigan), engineered mice lacking the gene for a sulfonylurea receptor known as SUR2. Although these mice initially appeared normal, they tended to die suddenly. The diabetes researchers wondered why.
So they began working with McNally, a specialist in cardiovascular genetics. McNally fitted the gene-altered mice with portable heart monitors, which revealed that they had elevated blood pressure and frequent cardiac “episodes.” About 50 times a day the mice had severe angina attacks, caused by spasms of their coronary arteries, which cut off the blood supply to the heart.
These repeated spasms, which lasted for several minutes, were often lethal. By the age of 30 weeks, 65 percent of male mice and 35 percent of females had died.
The spasms were caused by the missing receptor, the same one that is targeted by the sulfonylureas.
Sulfonylureas induce the pancreas to release insulin by blocking this receptor. Blocking the receptor inhibits a potassium channel on the cell surface. When this channel is closed, potassium ions build up in the cell, which eventually triggers the cell to open its calcium ion channels. Calcium flows in, which signals the cell to secrete insulin.
Unfortunately, a similar receptor exists on the smooth muscle cells that surround arteries, regulating flow through these vessels. The researchers found that mice without the receptor, had no functional potassium channels in their smooth muscle, leading to calcium influx and contraction of the smooth muscle cells that surround arteries.
Drugs that block calcium channels reduced the frequency of coronary episodes.
“We found that this receptor plays a pivotal role in the regulation of blood pressure and vascular tone,” said McNally. “The absence of the smooth muscle potassium channels promotes episodes of vascular spasm. Since the sulfonyureas work the same way, effectively closing these channels, we believe that they can increase susceptibility to vasospasm and therefore present a significant risk to diabetic patients. Since diabetic patients are already facing an increased risk of cardiovasculr disease, this is a further insult to their vessels.”
These gene-altered mice also provide an animal model of the disease known as Prinzmetal’s angina, which is caused by is coronary artery spasm. Unlike typical angina — chest pain during exertion — Prinzmetal’s nearly always occurs when a person is at rest.
“The good news,” adds McNally, “is that this study provides us with a new way to study Prinzmetal’s angina and suggests a molecular target for new drugs to treat hypertension and vasospasm.”
This research was supported by the National Institutes of Health, the American Heart Association and the Burroughs Wellcome Fund. Additonal researchers include William Chutkow and Matthew Wheeler of the University of Chicago; Jielin Pu, Tomoyuki and Jonathan Makielski of the University of Wisconsin; and Charles Burant of the University of Michigan.
Media Contact
More Information:
http://www.uchospitals.edu/All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
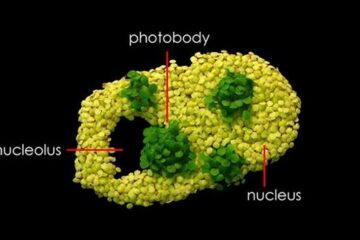
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…





















