Genetic Model for Devastating Form of Paraplegia Suggests New Treatments

A new genetic model for a motor disorder that confines an estimated 10,000 people in the United States to walkers and wheelchairs indicates that instability in the microscopic scaffolding within a key set of nerve cells is the cause of this devastating disability.
The study, which is published in the July 13 issue of the journal Current Biology, provides a provocative new insight into the molecular basis of the disease called hereditary spastic paraplegia (HSP) and suggests a new way to treat the inherited genetic disorder.
HSP—also known as familial spastic paraparesis and Strumpell-Lorrain syndrome—causes the ends of the nerves that control muscle activity to deteriorate. These nerve cells run from the brain’s cerebral cortex to the spinal cord where they connect to “downstream” nerve cells that excite muscles throughout the body to control coordinated movement. HSP causes weakness, spasms and loss of function in the muscles in the lower extremities.
More than 20 genes have been linked to HSP. However, more than 40 percent of all cases have been traced to a single gene (SPG4) that produces an enzyme called spastin. Previous studies have shown that this enzyme interacts with microtubules, the tiny protein tubes that provide structural support and transport avenues within most cells. Microtubules are dynamic structures, continually growing and shrinking, and their stability is closely regulated by a number of associated proteins. In nerve cells, microtubules carry cellular components to distant regions of the cell, regulate the growth of cellular branches and provide a substrate for important protein interactions. All of these functions are critically dependent on dynamic changes in microtubule stability.
Researchers in the laboratories of Kendal Broadie at Vanderbilt University and Andrea Daga at the University of Padova, Italy, collaborated on the first studies of the role that spastin plays in nerve communication in a living organism. They have discovered that spastin is highly enriched in nerve cells, especially in the synapses—the junctions between pairs of nerve cells and between nerve and muscle cells. Using advanced genetic engineering methods to manipulate gene dosage, their study showed that either too much or too little of the enzyme disrupts microtubule stability, degrading the nerve cells’ ability to function. They also found that pharmacological treatments that counteracted these destabilizing effects restored normal nerve function.
“These findings suggest that HSP is caused primarily through impaired regulation of the nerve cell cytoskeleton,” says Broadie, professor of biological sciences and pharmacology and an investigator at the Kennedy Center for Research on Human Development. “Spastin, as well as other HSP-linked genes, appears to mediate this common function. This suggests that treatment of this common defect may be effective for many, perhaps most, HSP patients.”
The organism that the researchers used in the study is the fruit fly, Drosophila melanogaster, the “lab rat” of genetics research. “Drosophila is the perfect organism to study complex genetic diseases like HSP,” says Vanderbilt graduate student Nick Trotta, who is the first author on the paper. “All we need to know is what gene is involved and we can change the way the gene is expressed within a few weeks. That lets us replicate the conditions associated with the disease so we can learn more about how it works.”
At the molecular level, there is very little difference between a Drosophila neuron and a human neuron, Trotta says. For example, fruit flies have a protein called D-Spastin that performs the same functions as human spastin. The two enzymes are 48 percent identical and 60 percent similar at the amino acid level.
“It may seem surprising that a fly can be used to uncover the molecular basis of human disease, but it has been shown over and over again in the last several decades that insights gained from Drosophila studies provide immediate insight into the human condition. There is a long history of Drosophila research pioneering major breakthroughs in our understanding of fundamental biological problems,” says Broadie.
To study how spastin functions in living neurons, the researchers designed transgenic flies with altered amounts of D-Spastin protein in their neurons and analyzed the effects.
Animals with lower levels of D-Spastin were weak, exhibited coordination defects and died prematurely. At the cellular level, the researchers found that the reduction of D-Spastin caused synapses to fill with ultra-stable microtubules. As a consequence, synapses were structurally reduced in size and showed profoundly altered communication properties.
Flies with heightened levels of D-Spastin were also sick. High levels of over-expression caused embryonic death. Lower levels caused nerve cell death (neurodegeneration.) Even very low levels of over-expression caused adults to be slow and weak. Within the nerve cells, the researchers found that too much D-Spastin caused stable microtubules to disappear altogether. At the synapse, elevated levels of spastin also caused a large drop in synaptic signal strength, impairing nerve communication.
These studies showed that spastin concentrates in synapses, where it acts locally to destabilize microtubules. Moreover, the researchers found that specific drugs that alter microtubule stability remedy the defects that occur in synaptic function as a result of changes in spastin levels. In both loss and over-expression cases, the researchers found that treatment with drugs that correct microtubule stability defects caused the synaptic signal strength to rebound to normal levels. This result suggests that drugs that stabilize microtubule activity might provide a new approach for treating HSP.
The Vanderbilt researchers were funded by the National Institutes of Health and the Italian researchers by the Telethon Foundation in Rome. Additional authors of the paper are Genny Orso and Maria Giovanna Rossetto from the University of Padova.
Media Contact
More Information:
http://www.vanderbilt.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
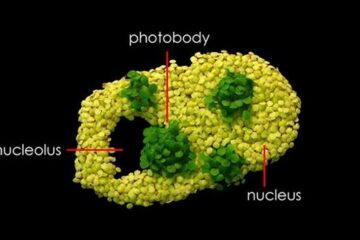
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…





















