Can an over-the-counter vitamin-like substance slow the progression of Parkinson's disease?

“At present, the very best therapies we have for Parkinson's can only mask the symptoms – they do not alter the underlying disease,” said neurologist Dr. Katie Kompoliti, a specialist in movement disorders. “Finding a treatment that can slow the degenerative course of Parkinsons's is the holy grail of Parkinson's research.”
The substance being tested, called coenzyme Q10, is produced naturally in the body and is an important link in the chain of chemical reactions that produce energy in mitochondria, the “powerhouses” of cells. The enzyme is also a potent antioxidant – a chemical that “mops up” potentially harmful chemicals generated during normal metabolism.
Several studies have shown that Parkinson's patients have impaired mitochondrial function and low levels of coenzyme Q10. Moreover, laboratory research has demonstrated that coenzyme Q10 can protect the area of the brain damaged in Parkinson's.
The Phase III clinical trial, a large, randomized study with a control group, follows an earlier investigation that tested several doses of coenzyme Q10 in a small group of patients with early-stage Parkinson's disease. The highest dose, 1,200 mg, appeared promising. Over the course of 16 months, patients taking this dose experienced significantly less decline than other patients in motor (movement) function and ability to carry out activities of daily living, such as feeding or dressing themselves.
But researchers involved in the study, including Kompoliti, were cautious about their findings, citing the need for a more extensive review to confirm the results.
In the present trial, funded by the National Institutes of Health and the National Institute of Neurological and Disorders and Stroke, 600 patients will be enrolled at 60 centers in the U.S. and Canada. Two dosages of coenzyme Q10 are being tested,1,200 mg and 2,400 mg, delivered in maple nut-flavored chewable wafers that also contain vitamin E.
Participants in the study will be evaluated periodically over 16 months for symptoms of Parkinson's disease, including tremor, stiffness of the limbs and trunk, impaired balance and coordination, and slowing of movements. They will also be assessed for ability to perform daily activities, overall quality of life, and need to take medications to alleviate symptoms.
About Rush:
Rush University Medical Center includes a 674-bed (staffed) hospital; the Johnston R. Bowman Health Center; and Rush University (Rush Medical College, College of Nursing, College of Health Sciences and the Graduate College).
Rush is currently constructing a 14-floor, 806,000-square-foot hospital building at the corner of Ashland Avenue and Congress Parkway. The new hospital, scheduled to open in 2012, is the centerpiece of a $1-billion, 10-year campus redevelopment plan called the Rush Transformation, which also includes a new orthopedics building (to open in Fall 2009), a new parking garage and central power plant completed in June 2009, renovations of selected existing buildings and demolition of obsolete buildings. The new hospital is being designed and built to conserve energy and water, reduce waste and use sustainable building materials. Rush is seeking Leadership in Energy and Environmental Design (LEED) gold certification from the U.S. Green BuildingCouncil. It will be the first full-service, “green” hospital in Chicago.
Rush's mission is to provide the best possible care for our patients. Educating tomorrow's health care professional, researching new and more advanced treatment options, transforming our facilities and investing in new technologies—all are undertaken with the drive to improve patient care now, and for the future.
Media Contact
More Information:
http://www.rush.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Simplified diagnosis of rare eye diseases
Uveitis experts provide an overview of an underestimated imaging technique. Uveitis is a rare inflammatory eye disease. Posterior and panuveitis in particular are associated with a poor prognosis and a…

Targeted use of enfortumab vedotin for the treatment of advanced urothelial carcinoma
New study identifies NECTIN4 amplification as a promising biomarker – Under the leadership of PD Dr. Niklas Klümper, Assistant Physician at the Department of Urology at the University Hospital Bonn…
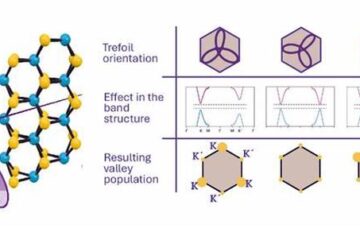
A novel universal light-based technique
…to control valley polarization in bulk materials. An international team of researchers reports in Nature a new method that achieves valley polarization in centrosymmetric bulk materials in a non-material-specific way…





















