Split-dose preparation for colonoscopy increases precancerous polyp detection rates

Colorectal cancer develops slowly, therefore screening for the disease is especially important. Colonoscopy screening allows for the detection and removal of precancerous polyps (small growths in the colon) during the same exam and before the polyps turn into cancer.
One of the most important steps in colonoscopy is patient bowel preparation. Adequate preparation ensures that the colon is thoroughly cleaned before the exam so that the physician can clearly see the entire colon to look for abnormalities, such as colon polyps, during the procedure. Cleansing the colon before a colonoscopy is called bowel preparation, or “prep.” It involves taking medication that causes diarrhea, emptying the colon. The medication is taken by mouth, and comes in liquid or tablet form. Patients also need to change what they eat during the day or two before the colonoscopy.
A good-quality bowel preparation is essential for colonoscopy to be effective. Inadequate bowel preparation can result in incomplete procedures, missed lesions, higher complication rates, and increased costs resulting from repeated procedures. The polyethylene glycol (PEG) solution is commonly used as a cleansing bowel preparation because it is safe and does not cause major fluid and electrolyte shifts. A major disadvantage, however, is the large volume required to be taken over a short time that may result in patient intolerance and poor compliance, leading to a poor preparation.
Recent studies have explored new approaches in administering PEG solutions to improve patient tolerability, compliance, and efficacy. Splitting the preparation is such an approach. Patients are advised to consume two or three liters the night before and one or two liters the morning of the procedure.
“A recent meta-analysis of randomized studies using split-dose preparations suggested a significant improvement in the quality of preparation and patient compliance. However, the effects of split-dose preparations on other quality indicators of colonoscopy, such as cecal intubation (colonoscopy completion) and adenoma detection rates, have not been evaluated, as far as we know,” said study lead author Suryakanth R. Gurudu, MD, Division of Gastroenterology and Hepatology, Mayo Clinic Arizona.
“In our study, we have demonstrated, for the first time to our knowledge, that system-wide implementation of a split-dose preparation for colonoscopy significantly improves both polyp detection rates and adenoma detection rates as well as improves the quality of the preparation and colonoscopy completion rates. These results confirm the benefit of split-dose preparations and the importance of bowel preparation in the detection of colon polyps.”
Methods
The primary aim of this study was to compare polyp detection rates (PDRs) and adenoma detection rates (ADRs) before and after implementation of split-dose preparations (SDP) as the preferred bowel preparation in a tertiary GI practice. Secondary goals were to compare the quality of the preparation and cecal intubation rates (colonoscopy completion rate) before and after implementation of the SDP. This was a retrospective study at Mayo Clinic Arizona. Electronic medical records of all the patients who underwent colonoscopy from January 2009 to December 2009 (before SDP) and from October 2010 to March 2011 (after SDP) were reviewed. All patients who underwent colonoscopy for screening and surveillance of colon polyps and cancer were included in the study.
The bowel preparation choices for split dosing were four-liter PEG electrolyte solution or MoviPrep (Salix Pharmaceuticals Inc., Raleigh, NC). Patients were instructed to avoid eating a high-fiber diet for two days before taking the bowel preparation and to drink only clear liquids for the entire day before colonoscopy. With the four-liter PEG solutions, patients were instructed to drink three liters the night before, starting at 6:00 pm, and one liter at least four hours before the scheduled procedure time on the day of the procedure. Patients using MoviPrep (after preparing the solution according to manufacturer's specifications) were instructed to drink half of the volume the night before colonoscopy, starting at 6:00 pm, and the other half at least four hours before the scheduled procedure time on the day of the procedure. All patients were instructed to take nothing by mouth for at least three hours before the procedure. Patients who had an early morning procedure or long travel time to the endoscopy unit were offered the option of taking the entire preparation the night before (nonsplit dose).
Results
After the application of exclusion criteria, there were 3,560 patients in the pre-SDP group and 1,615 patients in the post-SDP group. The pre-SDP and post-SDP patient groups were similar in age, body mass index, and gender. The mean ages of patients were 62 and 61 years, respectively, in the pre-SDP and post-SDP groups. SDP use increased significantly from 9 percent to 74 percent after implementation. In comparison with the pre-SDP group, both PDRs (44.1 percent to 49.5 percent) and ADRs (26.7 percent to 31.8 percent) significantly improved in the post-SDP group. The cecal intubation rate significantly increased from 93.6 percent to 95.5 percent in the post-SDP group.
Bowel preparation quality also improved significantly in the post-SDP group. The improvement was noted mainly in patients rated with good to excellent preparations (34.9 percent to 53.9 percent), at the expense of those rated with fair to adequate preparations (54.3 percent to 37.8 percent), and to a lesser degree in those with poor to inadequate preparations (10.6 percent to 8.3 percent).
Limitations noted by the researchers included the study's retrospective design and not all endoscopists were the same in both periods. Three endoscopists from the pre-SDP period left the institution and were replaced by five other endoscopists in the post-SDP period. The researchers concluded that system-wide implementation of split-dose preparation as the primary choice for colonoscopy significantly improved both PDRs and ADRs, overall quality of the preparation, and colonoscopy completion rates.
About the American Society for Gastrointestinal Endoscopy
Since its founding in 1941, the American Society for Gastrointestinal Endoscopy (ASGE) has been dedicated to advancing patient care and digestive health by promoting excellence and innovation in gastrointestinal endoscopy. ASGE, with more than 12,000 members worldwide, promotes the highest standards for endoscopic training and practice, fosters endoscopic research, recognizes distinguished contributions to endoscopy, and is the foremost resource for endoscopic education. Visit www.asge.org and www.screen4coloncancer.org for more information and to find a qualified doctor in your area.
About Endoscopy
Endoscopy is performed by specially-trained physicians called endoscopists using the most current technology to diagnose and treat diseases of the gastrointestinal tract. Using flexible, thin tubes called endoscopes, endoscopists are able to access the human digestive tract without incisions via natural orifices. Endoscopes are designed with high-intensity lighting and fitted with precision devices that allow viewing and treatment of the gastrointestinal system.
Media Contact
More Information:
http://www.asge.orgAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
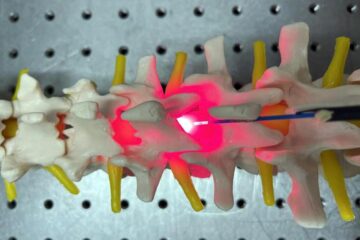
Red light therapy for repairing spinal cord injury passes milestone
Patients with spinal cord injury (SCI) could benefit from a future treatment to repair nerve connections using red and near-infrared light. The method, invented by scientists at the University of…

Insect research is revolutionized by technology
New technologies can revolutionise insect research and environmental monitoring. By using DNA, images, sounds and flight patterns analysed by AI, it’s possible to gain new insights into the world of…

X-ray satellite XMM-newton sees ‘space clover’ in a new light
Astronomers have discovered enormous circular radio features of unknown origin around some galaxies. Now, new observations of one dubbed the Cloverleaf suggest it was created by clashing groups of galaxies….





















