Mental disorders more prevalent in rural than urban settings in Mozambique

Advocacy to improve understanding of mental disorders, investment in mental-health resources in rural areas, and collaboration with traditional medical practitioners are urgently needed, especially in poor areas. These are the conclusions of authors of an Article in this week’s edition of The Lancet.
Dr Vikram Patel and Dr Helen Weiss, London School of Hygiene and Tropical Medicine, UK and colleagues studied 2739 households in Mozambique, 1796 in Maputo City and 943 in the rural town of Cuamba. A person from each household was asked to identify household members who had symptoms matching the three disorders above, as well as causes of the disorders, and their treatment and current state.
The researchers found that lifetime prevalence rates for all the three disorders were higher in rural than in urban settings. Prevalence of psychoses (in adults) was 4.4% in the rural town versus 1.6% in the city. For mental retardation, the prevalence was 1.9% (rural) versus 1.3 % (city), and for seizure disorders 4.0% (rural) versus 1.6% (city).
Informants in each house most frequently attributed psychoses to supernatural causes, followed by seizure disorder. In about three-quarters of all cases, households had consulted a traditional practitioner. Further, nearly half the people with these disorders in rural areas were rated as being in poor health.
The authors conclude: “These findings imply that mental-health policies in sub-Saharan Africa should focus on advocacy activities to raise awareness about severe mental and neurological disorders; investment in mental-health resources in community care settings, especially in rural areas; and close co-operation with traditional medical practitioners to promote recognition and appropriate management of people with severe mental and neurological disorders.”
In an accompanying Comment, Dr Julio Arboleda-Flórez, Ontario, Canada, says: “The results of this study should provide authorities in Mozambique, at whose behest the study was done, with a basis for planning health services…epidemiological and health-services research to determine the burden of mental illness are urgently needed in developing countries. The integration of mental health services into primary-care systems might be the only way to cope with that burden worldwide.”
Media Contact
More Information:
http://multimedia.thelancet.com/pdf/press/Mozambique.pdfAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
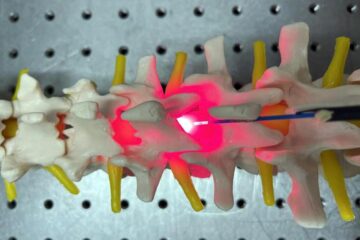
Red light therapy for repairing spinal cord injury passes milestone
Patients with spinal cord injury (SCI) could benefit from a future treatment to repair nerve connections using red and near-infrared light. The method, invented by scientists at the University of…

Insect research is revolutionized by technology
New technologies can revolutionise insect research and environmental monitoring. By using DNA, images, sounds and flight patterns analysed by AI, it’s possible to gain new insights into the world of…

X-ray satellite XMM-newton sees ‘space clover’ in a new light
Astronomers have discovered enormous circular radio features of unknown origin around some galaxies. Now, new observations of one dubbed the Cloverleaf suggest it was created by clashing groups of galaxies….





















