Draining away brain's toxic protein to stop Alzheimer's

That’s the method outlined in a paper published online August 12 by Nature Medicine. Scientists from the University of Rochester Medical Center show how the body’s natural way of ridding the body of the substance is flawed in people with the disease. Then the team demonstrated an experimental method in mice to fix the process, dramatically reducing the levels of the toxic protein in the brain and halting symptoms. The team is now working on developing a version of the protein that could be tested in people with the disease.
The approach doesn’t take direct aim at the pathology that is ubiquitous in the Alzheimer’s patients’ brains, where amyloid-beta forms a toxic plaque. Instead, researchers take an indirect approach, focusing not on the brain but rather on a protein that sops up amyloid-beta in the body, where it’s regarded as harmless. The scientists found that if they increase the body’s ability to soak up amyloid, the brain responds, causing levels of the substance in the brain – the real target – to plummet.
“There is a dynamic equilibrium between the levels of amyloid-beta in the blood and in the brain,” said neuroscientist Berislav Zlokovic, M.D., Ph.D., the leader of the team. “If we are able to lower the levels of amyloid-beta circulating in blood by sequestering more of it there, then the brain should follow and lower its levels too. This is exactly what we found.”
The team concentrated its efforts around a protein known as sLRP (soluble low-density lipoprotein receptor-related protein). The team discovered that in healthy people, the protein binds to and neutralizes anywhere from 70 to 90 percent of the amyloid-beta that is circulating in the body.
The team also found that sLRP is doing only a fraction of the job in Alzheimer’s patients that it does in healthy people. Levels of sLRP in people with Alzheimer’s were about 30 percent lower than in healthy people, and the sLRP that was present was almost three times as likely to be damaged compared to the same protein in healthy people. As a result, the Alzheimer’s patients had on average three to four times as much loose, unbound amyloid-beta floating in their bloodstreams – high levels that would likely also be reflected in the brain.
Zlokovic’s group decided to try to reduce amyloid-beta levels in the body by synthesizing an altered, super-potent form of sLRP that binds amyloid-beta more efficiently than natural sLRP. In blood samples from patients with Alzheimer’s disease, the modified version of sLRP, known as LRP-IV, soaked up and virtually eliminated amyloid-beta. The compound had an even more dramatic effect in mice with features of Alzheimer’s disease: LRP-IV lowered the levels of amyloid-beta in their brains by 85 to 90 percent. The mice that received the compound also had improved learning and memory compared to mice that did not receive LRP-IV, and they had 65 percent more blood flow in their brains in response to brain stimulation – a flick of their whiskers.
The team is now working with a company created by Zlokovic, Socratech, to create a form of LRP-IV that could be tested in people. Zlokovic hopes to have such a product ready for testing within two years.
Zlokovic, a scientist widely recognized for demonstrating that blood vessels, blood flow, and the blood-brain barrier are all central to the development of Alzheimer’s disease, likens the new approach to how statins help people with heart disease. Statins lower excess cholesterol in the bloodstream before the cholesterol can glom onto a blood vessel and cause problems with blood flow; in the same way, LRP-IV lowers amyloid-beta and indirectly lowers levels of amyloid-beta in the brain.
It was more than a decade ago that Zlokovic first identified LRP, a molecule that acts like an escort service in the brain, shuttling amyloid-beta out of the brain and into the body. The amyloid plaques that speckle the brains of Alzheimer’s patients are a hallmark of the disease, and where they come from and how to get rid of them has long been a focus of scientists.
“We used to think that Alzheimer’s disease was a problem with the production of too much amyloid-beta, but it’s become clear in recent years that the problem is with faulty clearance of amyloid-beta,” said Zlokovic, professor of Neurosurgery and Neurology and director of the Frank P. Smith Laboratory for Neuroscience and Neurosurgery Research. “We aren’t really talking about massive amounts of amyloid-beta. Even a small malfunction in the elaborate system that carries it into or out of the brain could lead, over years, to accumulate in amounts that damage the brain.”
Media Contact
More Information:
http://www.urmc.rochester.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
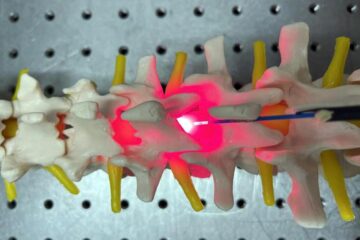
Red light therapy for repairing spinal cord injury passes milestone
Patients with spinal cord injury (SCI) could benefit from a future treatment to repair nerve connections using red and near-infrared light. The method, invented by scientists at the University of…

Insect research is revolutionized by technology
New technologies can revolutionise insect research and environmental monitoring. By using DNA, images, sounds and flight patterns analysed by AI, it’s possible to gain new insights into the world of…

X-ray satellite XMM-newton sees ‘space clover’ in a new light
Astronomers have discovered enormous circular radio features of unknown origin around some galaxies. Now, new observations of one dubbed the Cloverleaf suggest it was created by clashing groups of galaxies….





















