Researchers train the immune system to deliver virus that destroys cancer in lab models

An international team of researchers led by Mayo Clinic have designed a technique that uses the body’s own cells and a virus to destroy cancer cells that spread from primary tumors to other parts of the body through the lymphatic system. In addition, their study shows that this technology could be the basis for a new cancer vaccine to prevent cancer recurrence.
The study appeared in the Dec. 9 online issue of Nature Medicine.
The technology combines infection-fighting T-cells with the vesicular stomatitis virus that targets and destroys cancer cells while leaving normal cells unharmed. The study, which has not yet been replicated in humans, is significant because it describes a potential new therapy to treat and prevent the spread of cancer in patients.
“We hope to translate these results into clinical trials. However, until those trials are done, it’s difficult to be certain that what we see in mouse models will clearly translate to humans. We’re hopeful that will be the case,” says Richard Vile, Ph.D., a Mayo Clinic specialist in molecular medicine and immunology and the study’s principal investigator.
In primary cancers of the breast, colon, prostate, head and neck and skin, the growth of secondary tumors often pose the most threat to patients, not the primary tumor. The prognosis for these patients often depends upon the degree of lymph node involvement and whether the cancer has spread.
Dr. Vile and colleagues theorized that they could control the spread of cancer through the lymphatic system (bone marrow, spleen, thymus and lymph nodes) by manipulating the immune system.
Researchers zeroed in on immature T-cells from bone marrow, programming them to respond to specific threats to the immune system while delivering a cancer-destroying virus to the tumor cells.
To deliver the virus, researchers removed T-cells from a healthy mouse, loaded them with the virus and injected the T-cells back into the mouse. Researchers found that once the T-cells returned to the lymph nodes and spleen, the virus detached itself from the T-cells, found the tumor cells, selectively replicated within them and extracted tumor cells from those areas.
CANCER VACCINE
The procedure used in this study triggered an immune response to cancer cells, which means that it could be used as a cancer vaccine to prevent recurrence.
“We show that if you kill tumor cells directly in the tumor itself, you can get a weak immunity against the tumor, but if you use this virus to kill tumor cells in the lymph nodes, you get a higher immunity against the tumor,” Dr. Vile says.
RESULTS
The technique used in this study successfully treated the cells of three different diseases: melanoma, lung cancer and colorectal cancer. The results include:
Two days after treatment, the presence of melanoma tumor cells in lymph nodes was significantly less, but not completely gone. There were no cancer cells in the spleen.
Ten-to-14 days after a T-cell transfer, both the lymph nodes and spleen were free of melanoma tumor cells.
Mice treated with a single dose of the T-cells transfer developed a potent T-cell response against melanoma tumor cells.
Although the procedure was not intended to treat the primary melanoma tumor, significant reductions in tumor cells were observed.
In mice with lung cancer metastasis, cancer cells were significantly reduced in one-third of mice and completely eradicated in two-thirds of mice. Efforts to clear metastases from colorectal tumors were similarly effective.
Lung and colorectal tumor cells were purged from lymph nodes. Also, the spleens of mice that had lung cancer developed immunity to the cancer after the treatment.
The technology already exists to extract T-cells from patients, attach the virus and inject the cells back into the patients. Doctors currently use a similar process to attach radioactive tracers to T-cells when trying to find the source of an infection in patients.
“This is technology that is relatively easy to translate to humans because it involves taking T-cells from the patient — something routinely done today — loading them with this virus and then putting those T-cells back into patients whose cancer has spread to lymph nodes, are at high risk of the cancer spreading to other parts of the body or are at high risk of succumbing to the cancer,” Dr. Vile says.
Media Contact
More Information:
http://www.mayo.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
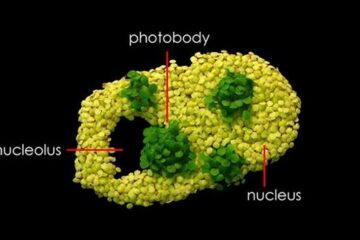
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…





















