Omega-3 fatty acids appear to impact AMD progression

The researchers calculated intakes of docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) from dietary questionnaires administered to 2,924 men and women, aged 55 to 80 years, participating in an eight-year supplement trial, the Age-Related Eye Disease Study (AREDS) of the National Eye Institute (NEI).
The AREDS trial results suggest taking supplements of antioxidants plus zinc prevents progression of late-stage AMD. AREDS study participants were randomly allocated to receive either a placebo or supplements containing the antioxidants vitamins C and E and beta carotene, the minerals zinc and copper, or a combination of both.
“In our study, we observed participants with early stages of AMD in the placebo group benefited from higher intake of DHA, but it appears that the high-dose supplements of the antioxidants and/or the minerals somehow interfered with the benefits of DHA against early AMD progression,” says senior author Allen Taylor, PhD, director of the LNVR at the USDA HNRCA. Taylor is also a professor at the Friedman School of Nutrition Science and Policy at Tufts and Tufts University School of Medicine (TUSM).
The antioxidant supplements did not seem to interfere with the protective effects of DHA and EPA against progression to advanced stages of AMD. Participants who consumed higher amounts of DHA and EPA appeared to have lower risk of progression to both wet and dry forms of advanced AMD. The results are published on-line ahead of print in the British Journal of Ophthalmology.
“Data from the present study also shows the supplements and omega-3 fatty acids collaborate with low-dietary glycemic index (dGI) diets against progression to advanced AMD,” says corresponding author Chung-Jung Chiu, DDS, PhD, a scientist in the LNVR and an assistant professor at TUSM. “Our previous research suggests a low-GI diet may prevent AMD from progressing to the advanced stage. We hypothesize that the rapid rise of blood glucose initiated by high-GI foods results in cellular damage that retinal cells cannot handle, thus damaging eye tissues.”
dGI is a scale used to determine how quickly carbohydrates are broken down into blood sugar, also known as blood glucose. Foods such as sweetened drinks, sodas and white bread are high-GI because they trigger a sharp rise and fall of blood sugar. Low-GI foods, such as whole grain versions of pasta and bread, have a milder effect on blood sugar response. Earlier data published by Taylor and Chiu suggests that daily substitution of five slices of whole grain bread for white bread out of a total intake of 250 g of carbohydrate might cut out almost 8% of advanced AMD over five years. This is readily achievable with little diet behavior modification.
Eating two to three servings of fatty fish such as salmon, tuna, mackerel, shellfish, and herring every week would achieve the recommended daily intake of DHA and EPA. However, the majority of AREDS participants and Americans eat a much lower level than recommended. “If changing dietary habits is not easy, supplementation is an option,” says Chiu.
The authors stress it is still premature to conclude dietary recommendations for people with AMD and more studies are warranted. “Taken together, these data indicate that consuming a diet with higher levels of omega-3 fatty acids, antioxidants and low-GI foods may delay compromised vision due to AMD,” says Taylor. “The present study adds the possibility that the timing of a dietary intervention as well as the combination of nutrients recommended may be important.”
AMD is a progressive disease that attacks central vision, resulting in a gradual loss of eyesight and, in some cases, blindness. The NEI reports that AMD is the most common causes of non-remediable vision loss in Americans over 60.
The study was awarded The Association for Research in Vision and Ophthalmology (ARVO)-American Foundation for Eye Research (AFER)/Merck Innovative Ophthalmology Research Award at the ARVO 2009 Annual Conference in May. The award is given to researchers under 45 to encourage research leading to improved quality of life for patients.
The authors received funding for this study from the following: United States Department of Agriculture (USDA), the National Institutes of Health, the Johnson & Johnson Focused Giving Program, the American Health Assistance Foundation and the Ross Aging Initiative.
About Tufts University School of Nutrition
The Gerald J. and Dorothy R. Friedman School of Nutrition Science and Policy at Tufts University is the only independent school of nutrition in the United States. The school's eight degree programs which focus on questions relating to famine, hunger, poverty, and communications, are renowned for the application of scientific research to national and international policy. For two decades, the Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University has studied the relationship between good nutrition and good health in aging populations. Tufts research scientists work with federal agencies to establish the USDA Dietary Guidelines, the Dietary Reference Intakes, and other significant public policies.
If you are a member of the media interested in learning more about this topic, or speaking with a faculty member at the Friedman School of Nutrition Science and Policy at Tufts University, or another Tufts health sciences researcher, please contact Andrea Grossman at 617-636-3728 or Christine Fennelly at 617-636-3707.
Media Contact
More Information:
http://www.tufts.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
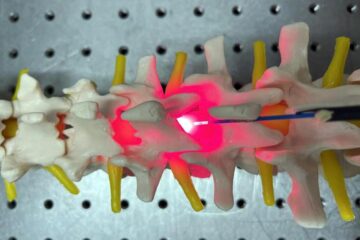
Red light therapy for repairing spinal cord injury passes milestone
Patients with spinal cord injury (SCI) could benefit from a future treatment to repair nerve connections using red and near-infrared light. The method, invented by scientists at the University of…

Insect research is revolutionized by technology
New technologies can revolutionise insect research and environmental monitoring. By using DNA, images, sounds and flight patterns analysed by AI, it’s possible to gain new insights into the world of…

X-ray satellite XMM-newton sees ‘space clover’ in a new light
Astronomers have discovered enormous circular radio features of unknown origin around some galaxies. Now, new observations of one dubbed the Cloverleaf suggest it was created by clashing groups of galaxies….





















