Non-endoscopic migraine surgery provides significant symptom relief

A revised version of a surgical procedure to treat severe chronic migraine headaches led to significant symptom relief more than 90 percent of the time in patients treated at Massachusetts General Hospital (MGH). Physicians from the MGH Division of Plastic and Reconstructive Surgery report that more than half of 35 patients treated with the non-endoscopic procedure – all of whom had headaches associated with compression of craniofacial nerves – reported complete symptom relief a year later. The team's paper has received advance online publication in the journal Plastic and Reconstructive Surgery.
“We confirmed that surgery through standard incisions used for cosmetic procedures can be very effective in treating some of the most severe cases of chronic migraine,” says William G. (Jay) Austen, Jr., MD, chief of Plastic and Reconstructive Surgery at MGH, who led the study. “While the earlier version of this procedure used an endoscope, not every patient is a candidate for endoscopic surgery, and not every surgeon has access to or experience with the equipment. We hope that this may increase the availability of this treatment.
Surgical treatment of migraine headaches was developed by Cleveland plastic surgeon Bahman Guyuron, MD, who had observed that some patients receiving cosmetic procedures of the forehead also had relief of migraine symptoms. Several studies by Guyuron and other investigators have supported the hypothesis that compression of the trigeminal and other craniofacial nerves can be an important trigger for migraine symptoms in some patients. The temporary symptom relief some patients experience through injections of botulinum toxin (Botox), which would release pressure from overactive muscles, further supports the theory.
Although Guyuron's original version of this procedure almost always used an endoscope to access and remove muscles contracting around specific nerves, the MGH team and other investigators have focused on developing ways to access migraine trigger points – specific sites of nerve compression that differ from patient to patient – through open incisions used in several cosmetic procedures.
Patients included in the current study all had chronic migraines that had been confirmed by a full neurological exam and had not responded to standard medical therapies. Previous symptom relief from treatment with Botox or nerve blocks, which would support a role for nerve compression, was required for inclusion in the study. Trigger points were identified based on patients' symptoms and histories, including response to previous procedures; and surgery was performed to free those sites from compressing muscles, connective tissue, blood vessels or bony structures.
The study analyzed a total of 43 procedures performed on 35 patients. Of those procedures, 90.1 percent resulted in symptom resolution – defined as a greater than 50 percent improvement in the frequency, duration and severity of migraine pain. Complete elimination of migraine symptoms was produced by 51.3 percent of successful procedures; 28.2 percent resulted in a greater than 80 percent improvement, and 20.5 percent produced a 50 to 80 percent improvement.
Austen stresses that selecting the appropriate patients for this procedure – including preliminary evaluations by a neurologist specializing in migraines – is essential. “We're still at the early stages of developing this concept and are now conducting a prospective study to find better ways of evaluating which patients we can help. We need to develop more evidence that this approach will be successful in the hands of surgeons at many different centers. No one is claiming that this is a cure for migraines, but the results of our study and others clearly indicate that this procedure can make a big difference in the lives of the right patients.”
Austen is an associate professor of Surgery at Harvard Medical School. Co-authors of the paper are Lisa Gfrerer, MD, lead author; Daniel Maman, MD, and Oren Tessler, MD, all of the MGH Division of Plastic and Reconstructive Surgery. The manuscript version of the report is currently available at http://journals.lww.com/plasreconsurg/Abstract/publishahead/Non__Endoscopic_Deactivation_of_Nerve_Triggers_in.99477.aspx.
Massachusetts General Hospital, founded in 1811, is the original and largest teaching hospital of Harvard Medical School. The MGH conducts the largest hospital-based research program in the United States, with an annual research budget of more than $785 million and major research centers in HIV/AIDS, cardiovascular research, cancer, computational and integrative biology, cutaneous biology, human genetics, medical imaging, neurodegenerative disorders, regenerative medicine, reproductive biology, systems biology, transplantation biology and photomedicine.
Media Contact
More Information:
http://www.massgeneral.org/All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
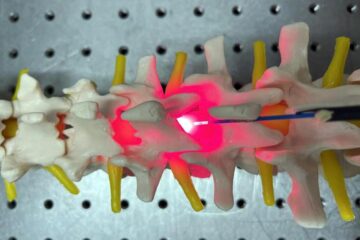
Red light therapy for repairing spinal cord injury passes milestone
Patients with spinal cord injury (SCI) could benefit from a future treatment to repair nerve connections using red and near-infrared light. The method, invented by scientists at the University of…

Insect research is revolutionized by technology
New technologies can revolutionise insect research and environmental monitoring. By using DNA, images, sounds and flight patterns analysed by AI, it’s possible to gain new insights into the world of…

X-ray satellite XMM-newton sees ‘space clover’ in a new light
Astronomers have discovered enormous circular radio features of unknown origin around some galaxies. Now, new observations of one dubbed the Cloverleaf suggest it was created by clashing groups of galaxies….





















