Discovery may help prevent chemotherapy-induced anemia

Now, researchers at Albert Einstein College of Medicine of Yeshiva University have discovered that chemo also induces an insidious type of nerve damage inside bone marrow that can cause delays in recovery after bone marrow transplantation.
The findings, made in mice and published online today in Nature Medicine, suggest that combining chemotherapy with nerve-protecting agents may prevent long-term bone marrow injury that causes anemia and may improve the success of bone marrow transplants.
Constantly regenerating and maturing, the hematopoietic (blood-producing) stem cells in our bone marrow produce billions of red blood cells (RBC) every day. Cancer chemotherapy is notorious for injuring the bone marrow, leading to anemia, or low RBC counts. But just how chemotherapy harms the bone marrow has not been clear.
Anemia can lead to numerous health problems including chronic fatigue, tachycardia (abnormally rapid heartbeat), cognitive impairment, shortness of breath, depression and dizziness. In addition, studies have shown that cancer patients who develop anemia have a 65 percent increased risk of death compared with cancer patients without anemia.
In an earlier study, senior author Paul Frenette, M.D., professor of medicine and of cell biology and director of the Ruth L. and David S. Gottesman Institute for Stem Cell and Regenerative Medicine Research at Einstein, found that sympathetic nerves within bone marrow direct the movement of hematopoietic stem cells. (The body's sympathetic nervous system helps in controlling most internal organs—increasing heart rate and dilating the pupils of the eye, for example.)
“Since many chemotherapies used in cancer treatment are neurotoxic, we wondered whether they might also damage sympathetic nerves in bone marrow itself, impairing the ability of hematopoietic cells to regenerate and to manufacture RBCs,” said Dr. Frenette. “This possibility hadn't been examined before.”
Dr. Frenette and his colleagues treated mice with seven cycles of cisplatin, a common chemotherapy drug with known neurotoxic effects. The cisplatin caused peripheral neuropathy problems similar to those seen in cancer patients. The mice were then given fresh bone marrow transplants to see how well their marrow would regenerate. Despite receiving fresh stem cells, the cisplatin-treated mice had delayed recovery of blood counts compared to controls—suggesting that the prior cisplatin treatments had affected the bone marrow and prevented hematopoietic stem cells from regenerating. By contrast, mice treated with carboplatin—a non-neurotoxic chemotherapy—recovered their ability to produce blood after bone marrow transplantation.
To confirm that healthy sympathetic nerves in the bone marrow are needed to regenerate hematopoietic stem cells and produce RBCs, the researchers selectively damaged sympathetic nerves in bone marrow using chemicals or genetic engineering. In both cases, the mice with the damaged sympathetic nerves were less able than control mice to recover after bone marrow transplant.
The researchers found that injury to these nerves could be reduced by giving mice nerve-protecting agents along with chemotherapy. Mice treated with seven cycles of cisplatin along with 4-methylcatechol (an experimental drug that reportedly protects sympathetic nerves) showed improved response to bone marrow transplantation, compared to controls.
Dr. Frenette and his colleagues now plan to look for compounds that can protect sympathetic nerves in the bone marrow without reducing the effectiveness of cancer chemotherapies.
The title of the paper is “Chemotherapy-induced bone marrow nerve injury impairs hematopoietic regeneration.” The lead author of the paper is Daniel Lucas, Ph.D., a postdoctoral reseacher in Dr. Frenette's laboratory. Other Einstein contributors are Christoph Scheiermann, Ph.D., and Yuya Kunisaki, M.D., Ph.D. Additional co-authors are Andrew Chow, M.D./Ph.D. student, Icahn School of Medicine at Mount Sinai, New York, NY; Ingmar Bruns, M.D., Ph.D., Einstein and Heinrich Heine University, Dusseldorf, Germany; Colleen Barrick, National Cancer Institute, Frederick, MD; and Lino Tessarollo, Ph.D., National Cancer Institute.
This work was supported by grants from the National Institute of Diabetes and Digestive and Kidney Diseases (DK056638) and the National Heart, Lung, and Blood Institute (HL069438), both parts of the National Institutes of Health.
A patent application on this technology has been filed, which is currently available for licensing and further commercialization.
The authors declare no competing financial interests.
About Albert Einstein College of Medicine of Yeshiva University
Albert Einstein College of Medicine of Yeshiva University is one of the nation's premier centers for research, medical education and clinical investigation. During the 2012-2013 academic year, Einstein is home to 742 M.D. students, 245 Ph.D. students, 116 students in the combined M.D./Ph.D. program, and 360 postdoctoral research fellows. The College of Medicine has more than 2,000 full-time faculty members located on the main campus and at its clinical affiliates. In 2012, Einstein received over $160 million in awards from the NIH. This includes the funding of major research centers at Einstein in diabetes, cancer, liver disease, and AIDS. Other areas where the College of Medicine is concentrating its efforts include developmental brain research, neuroscience, cardiac disease, and initiatives to reduce and eliminate ethnic and racial health disparities. Its partnership with Montefiore Medical Center, the University Hospital and academic medical center for Einstein, advances clinical and translational research to accelerate the pace at which new discoveries become the treatments and therapies that benefit patients. Through its extensive affiliation network involving Montefiore, Jacobi Medical Center –Einstein's founding hospital, and five other hospital systems in the Bronx, Manhattan, Long Island and Brooklyn, Einstein runs one of the largest residency and fellowship training programs in the medical and dental professions in the United States. For more information, please visit http://www.einstein.yu.edu and follow us on Twitter @EinsteinMed.
Media Contact
More Information:
http://www.einstein.yu.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
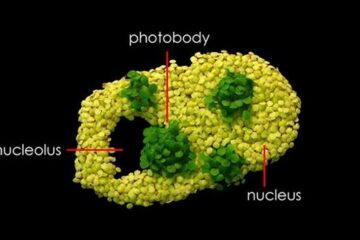
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…





















