Cancer scientists discover new way breast cancer cells adapt to environmental stress

The findings, published today in Genes and Development (http://www.genesdev.org/cgi/doi/10.1101/gad.1987211), show how breast cancer cells can thrive when deprived of their usual diet of glucose (sugar) and oxygen by turning to fatty acids for energy generation.
“Our results demonstrate that a protein not previously associated with breast cancer is involved in helping these cells to adapt to starvation conditions and to continue their uncontrolled growth,” says Dr. Mak, principal investigator and Weekend to End Breast Cancer Chair in Breast Cancer Research at PMH. Dr. Mak is also a Professor at the University of Toronto in the Departments of Medical Biophysics and Immunology.
In the lab, researchers used an anticancer drug called rapamycin to block a molecular signalling pathway within breast cancer cells that stimulates sugar metabolism. However, instead of dying of starvation, the cells continued to multiply. The team also observed an increase in these cells of carnitine palmitoyltransferase 1C (CPT1C), a protein usually found only in the brains of healthy individuals. Moreover, cells engineered to produce high levels of CPT1C were also able to adapt their metabolism as a survival technique.
“In other words,” says Dr. Mak, “The cancer cells acted like cheaters on a diet and found a new food source in fatty acids.
“The fact that CPT1C becomes expressed under conditions of metabolic stress highlights the resilience of cancer cells. They are able to adapt to environmental challenges and find alternative sources of food in order to flourish where healthy cells would not survive.”
“Our discovery that deprivation of either sugar or oxygen spurs CPT1C expression in tumour cells marks this protein as a potential target for new drug development,” says Dr. Mak.
“We also demonstrated that cells that were prevented from using CPT1C to cope with a disruption in sugar metabolism became more sensitive to environmental stress. These findings represent an important stepping stone to developing targeted therapies that can block cancer cells from adapting to environmental challenges and surviving efforts to kill them.”
This most recent discovery builds on Dr. Mak's impressive body of work, which has led to important breakthroughs in immunology and our understanding of cancer at the molecular level. Dr. Mak is internationally renowned for his 1984 landmark scientific paper on the cloning of the genes for the T cell receptor, a key component of the human immune system.
The research published today was financially supported by grants from the Canadian Institutes of Health Research, The Princess Margaret Hospital Foundation, The Canadian Cancer Society, the Forschungskredit of the University of Zurich and Oncosuisse.
About The Campbell Family Institute for Breast Cancer Research
The Campbell Family Institute for Breast Cancer Research at Princess Margaret Hospital brings together an elite team of cancer researchers, scientists, clinicians and staff dedicated to the ultimate goal of conquering breast cancer by leveraging basic, translational and clinical research into dramatic breast cancer breakthroughs. www.campbellfamilyinstitute.ca
About Princess Margaret Hospital, University Health Network
Princess Margaret Hospital and its research arm, Ontario Cancer Institute, have achieved an international reputation as global leaders in the fight against cancer. The Campbell Family Institute for Breast Cancer Research is the newest component of the Ontario Cancer Institute. It aims to become a world-leading program in breast cancer research by leveraging basic, translational, and clinical research into dramatic breast cancer breakthroughs. Princess Margaret Hospital is a member of the University Health Network, which also includes Toronto General Hospital and Toronto Western Hospital. All three are teaching hospitals affiliated with the University of Toronto. For more information, go to www.uhn.ca
Media Contact
More Information:
http://www.uhn.caAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…
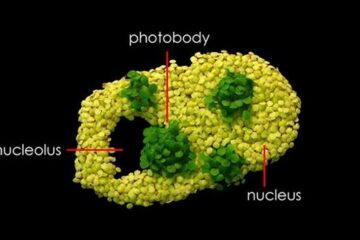
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…





















