New biomarkers for improving treatment of spondylarthritis

Clinical trials are essential to the development of effective treatments for chronic autoimmune arthritis. For ethical, practical, and financial reasons, researchers increasingly face the challenge of achieving proof-of-concept in early-phase clinical trials of limited size, limited duration, and minimal patient risk. Analysis of tissue from the synovium, the thin membrane lining the joint space and primary target of inflammation, provides a straightforward way to meet this challenge. This approach has been used extensively, and proven valuable, in studies of rheumatoid arthritis (RA).
Spondylarthritis (SpA) refers to a group of chronic autoimmune arthritic conditions, including ankylosing spondylitis (AS) and the arthritis associated with psoriasis and inflammatory bowel diseases, primarily affecting peripheral joints. For an international alliance of researchers, synovial tissue analysis presented an ideal vehicle for identifying biomarkers of SpA. Their findings, featured in the June 2006 issue of Arthritis & Rheumatism (http://www.interscience.wiley.com/journal/arthritis), hold the promise to facilitate the progress of clinical trials dedicated to improving the treatment of SpA.
Led by Dr. Dominique Baeten at the University of Amsterdam’s Academic Medical Center, the 12-week study included 52 patients who met established criteria for SpA. Patients were randomly divided into three groups. Two groups were treated with a tumor necrosis factor (TNFá) blockade – 20 received infliximab and 20 received etanercept. None of these 40 patients was being treated with a disease-modifying antirheumatic drug (DMARD). The remaining 12 patients served as controls. At the study’s inception and again at its culmination, each patient participated in a thorough assessment of disease symptoms and pain.
At the same intervals, weeks 0 and 12, synovial biopsies were performed on each patient, through needle arthroscopy of the knee. The synovial tissue samples were then subjected to extensive evaluation. The laboratory tests included measures of abnormal cell growth in the lining layer, vascular growth, markers of cellular infiltration, and metalloproteinases (MMPs) in the lining and sub-lining layers.
In both the anti-TNFá treatment groups, patients experienced significant improvements in disease activity, pain, and swollen and tender joint counts. In contrast, there was no improvement in the control group; in fact, there was a significant deterioration in patient assessment of pain. But the most noteworthy findings came from the analysis of whether changes in synovial tissue correlated with changes in disease activity between patients who had received effective treatment and those who had not.
Among the synovial features linked to anti-TNFá effectiveness, the researchers found changes in subsets of synovial macrophages, a type of white blood cell; changes in the levels of polymorphonuclear (PMN) cells, which work to fight infection; and changes in MMP-3 expression. Taken together, these findings indicate that, for SpA patients in particular, changes in disease activity are accompanied by series of distinct and measurable events in the peripheral joint.
To affirm these findings and strengthen their clinical application, the researchers also found that the same synovial features showed a highly different standardized response means between SpA patients receiving effective treatment and control patients. In validation analyses with independent synovial tissue samples, effective treatment was correctly predicted in 24 of 30 SpA patients.
As Dr. Baeten observes, these tiny changes in synovial tissue have the potential to be a great research and therapeutic asset. “Their ability to correctly discriminate between effective and ineffective treatment in small patient cohorts makes than interesting biomarkers to facilitate conclusive early phase clinical trials in SpA,” he notes. “Further studies are needed to confirm their value as biomarkers at early time points across different therapeutic regimens and to combine synovial assessment with predictors of axial response to treatment in SpA.”
Media Contact
All latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
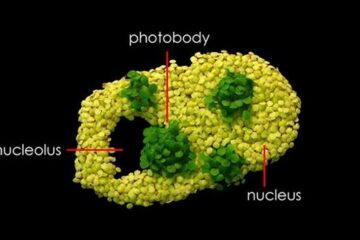
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…