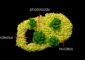
Researchers find that combined gene therapy eliminates glioblastoma multiforme in lab studies

Despite aggressive treatment, glioblastoma multiforme (GBM) – the most common and deadly of brain cancers – usually claims the lives of its victims within six to 12 months of diagnosis. Because GBM is so aggressive, the disease has been the target of a number of laboratory and clinical studies investigating the effectiveness of gene therapy to deliver novel therapies to the brain. In laboratory studies, this type of gene therapy has proved almost completely effective. But in clinical trials, it has had limited effectiveness.
To overcome these limitations, researchers at Cedars-Sinai Medical Center developed a large brain tumor model in laboratory rats that would more accurately predict the outcome of gene therapies in patients. In addition, they tested a genetically engineered virus to deliver two proteins directly to the brain. Their findings, reported in the August 15th issue of the journal Cancer Research, show that the majority of rats bearing large tumors were still alive six months after combined treatment with two proteins: RAdTK, a protein that kills cancer cells, and RAdFlt3L, which stimulates immune or dendritic cells in the brain.
“Our study shows that GBM tumors were completely eliminated in lab rats, likely because the two proteins increase the production of fully mature immune cells within the brain,” said Maria Castro, Ph.D., co-director of the Gene Therapeutics Research Institute at Cedars-Sinai Medical Center and the senior author of the study. “This suggests that combined RAdFlt3L and RAdTK gene therapy may ultimately provide an effective treatment for patients undergoing clinical trials with GBM.”
GBM tumors derive from brain astrocytes, a cell that normally supports and nurtures the brain’s neurons. GBM grows quickly, often becoming very large before any symptoms are experienced. Once GBM is diagnosed, conventional treatment begins with surgery to remove as much of the tumor as possible and is then followed with radiation and/or chemotherapy to slow progression of the disease. But despite aggressive treatment, the tumors recur and patients usually die within a year’s time.
To find another way to more effectively treat GBM, scientists have begun investigating the use of gene therapy to deliver novel therapeutic agents directly to the brain. Typically, these studies have tested the use of the suicide gene from the herpes simplex virus to develop a gene therapy approach that kills cancer cells in the presence of the antiviral drug – gancyclovir. In laboratory studies, this type of gene therapy has proved almost 100 percent effective. But in clinical trials, it has had limited effectiveness, suggesting that the tumor mass is too large for the gene to effect long-term.
“Because we haven’t seen the same positive results with gene therapy in clinical trials that we’ve seen treating GBM in laboratory rats, we realized that we needed to design a better model that more closely mimicked these tumors in patients,” Castro said. “We also wanted to test whether a combined gene therapy strategy using proteins known to kill cancer cells or promote an immune response would work to eliminate these larger tumors in the rats.”
Gene therapy is an experimental treatment that uses genetically engineered viruses to transport genes and/or proteins into cells. Just like a viral infection, the viruses work by tricking cells into accepting them as part of their own genetic coding. To make them safe, scientists remove the genetic viral genes that cause infection and engineer them so that they stop reproducing after they have delivered the therapeutic genes.
In this study, the researchers first developed a large GBM tumor model and implanted them in rats, allowing the tumor to grow for 10 days, when they were at their largest. Secondly, the investigators tested the effectiveness of various gene therapies used in combination or individually to see whether they would shrink or eliminate tumors.
To determine whether the size of the tumor significantly affected survival, the researches implanted both large and smaller GBM tumors in rats. The investigators then treated rats bearing GBM tumors with single or combined gene therapies (RAdTK and/or RAdFlt3l), or a saline placebo, as a control. They found that RAdTK treatment was 100 percent effective when delivered into small tumors, but only 20 percent effective when injected into large tumors. RAdFlt3L, on the other hand, was 60 percent effective if delivered into small tumors, but failed completely if injected into the large tumors. But when both RAdTK and RAdFlt3l were given in combination, the investigators found 70 percent of rats were still alive after six months of treatment and that the large GBM tumors had completely disappeared or shrank significantly.
“Just as with patients, our results emphasize that tumor size at the time of treatment is critical to predict clinical outcome,” said Pedro Lowenstein, M.D., Ph.D., director of the Gene Therapeutic Research Institute at Cedars-Sinai. “Our model reproduces more closely the human disease condition where tumor size at the time of treatment determines how well the patient will respond to therapies.”
“Our results show for the first time, that we could elicit a potent and stable anti-tumor immune response in the brains of rats bearing large GBM tumors,” Castro said. “In these pre-clinical studies, combined gene therapy treatment with RAdTK and RAdFlt3L dramatically increased survival, without adverse immune reactions in the brain.”
Media Contact
All latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
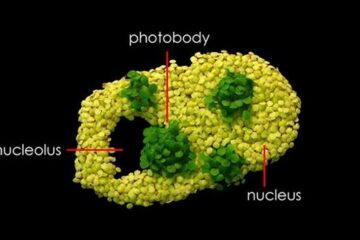
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…