Gene Therapy That Overcomes Blood-Brain Barrier to Treat Central Nervous System Manifestations

Mucopolysaccharidosis (MPS) type VII (also known as Sly syndrome) is a lysosomal storage disorder (LSD) characterized by a deficiency of the lysomal enzyme beta-glucuronidase. MPS VII leads to bone and joint abnormalities, enlargement of the visceral organs, cardiovascular disease and neurologic impairment. Using a MPS VII adult animal model, researchers in the Center for Gene Therapy at Columbus Children’s Research Institute (CCRI) on the campus of Columbus Children’s Hospital have demonstrated a gene therapy strategy whereby in vivo administration into the liver of a recombinant adeno-associated virus (rAAV) type 2 vector is capable of reversing the progression of storage in the liver, spleen, kidney, heart, lung and, importantly, the brain. This is the first time researchers have demonstrated that the peripheral in vivo administration of a therapeutic gene leads to improvement in the brain of an adult MPS VII animal model. The findings were published in the September issue of Molecular Therapy.
Previous work has shown that similar therapies are effective in treating the brain if administered soon after birth, but until now, it was believed that the blood-brain barrier would prevent this occurrence during adulthood.
“It’s not clearly understood why in newborns, the blood-brain barrier is ‘open,’ and as a person matures, very few substances can cross through this barrier,” said Thomas J. Sferra, M.D., gastroenterologist and associate professor at The Ohio State University College of Medicine and Public Health. “In our study, we were able to show an improvement in the manifestations of this disease within the brain. Now that we have proven that this type of therapy can overcome the blood-brain barrier, we can begin to study how this occurred. In the long-term, we have the potential to apply this type of therapy to a majority of the LSDs and even other disorders.”
Lysosomes are described as the cell’s “recycling center,” whereby enzymes continuously breakdown large molecules into smaller materials to be reused by the cell. LSDs are inherited disorders caused by a deficiency of one of the lysosomal enzymes. This deficiency interferes with the normal breakdown process causing an accumulation of abnormal molecules in the lysosomes. This accumulation prohibits normal function of the particular organ (such as the liver, spleen, bone, and brain) in which the storage occurs. There are more than 40 types of LSDs and the combined incidence of these diseases is one in every 8,000 live births.
For his research, Sferra conducted two studies in adult MPS VII animal models to test the effect of different amounts of the rAAV vector and to analyze the length of time for improvement of the disease to begin. To achieve the highest level of gene transfer upon administration, the vector was injected directly into the liver.
“After a single administration of the rAAV vector, we observed a reduction of lysosomal storage in every organ analyzed at two months post-injection. Importantly, this disease improvement was maintained for at least one year after vector administration,” said Sferra.
Currently, Sferra’s team is engaged in early studies using the rAAV vector as a transport mechanism to carry genes to treat other diseases.
Columbus Children’s ranks among the top 10 in National Institutes of Health research awards and grants to freestanding children’s hospitals in the country and houses the Department of Pediatrics of The Ohio State University College of Medicine and Public Health. With nearly 600,000 patient visits each year, Children’s Hospital is a 112-year-old pediatric healthcare network treating newborns through age 21. In 2003, the Columbus Children’s Research Institute conducted more than 300 research projects and is the home of Centers of Emphasis encompassing gene therapy; molecular and human genetics; vaccines and immunity; childhood cancer; cell and vascular biology; developmental pharmacology and toxicology; injury research and policy; biopathology; microbial pathogenesis; and biobehavioral health. Pediatric Clinical Trials International (PCTI), a site management organization affiliated with the hospital, also coordinated more than 50 clinical trials. In addition to having one of the largest ambulatory programs in the country, Children’s offers specialty programs and services. More than 75,000 consumers receive health and wellness education each year and affiliation agreements with nearly 100 institutions allow more than 1,700 students and 500 residents to receive training at Children’s annually. More information on Children’s Hospital of Columbus is available by calling (614) 722-KIDS (5437) or through the hospital’s Web site at http://www.columbuschildrens.com.
Media Contact
More Information:
http://www.columbuschildrens.comAll latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
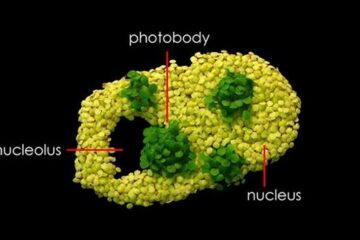
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…