Interferon Needed for Cells to 'Remember’ How to Defeat a Virus

The findings, available online and in the Dec. 15 issue of the Journal of Immunology, have potential application in the development of more effective vaccines and anti-viral therapies.
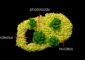
Typically, when a person is infected with a virus, the human body immediately generates a massive number of T cells – a type of immune cell – that kill off the infected cells. Once the infection has cleared, most of the T cells also die off, leaving behind a small pool of central memory cells that “remember” how to fight that particular type of virus if the person is infected again.
“In this study, we have uncovered interferon’s role and the key signaling protein, called IL-2, involved in generating memory T cells,” said Dr. David Farrar, assistant professor of immunology at UT Southwestern and senior author of the study. “Knowing how T cells acquire this memory may help us design better strategies and vaccines to fight HIV and other infectious diseases. Further, our discovery was made using primary human CD4+ T cells, which underscores the relevance of our discovery to human immune responses.”
CD4+ T cells coordinate the actions of other cells at the site of infection.
When a virus or bacterium infects a human, the infected cells secrete several molecules, including a cytokine – or signaling protein – called interferon alpha. The action of interferon is what makes an infected person feel run down and tired. Although scientists knew that interferon alpha prevented a virus from multiplying and spreading, they didn’t know what role interferon played in the creation of memory cells.
In the current study, the UT Southwestern researchers show that both interferon alpha and another signaling protein called IL-12 are needed to induce the creation of memory cells. They found that interferon and IL-12 team up to promote the creation of a special set of cells that then secrete another signaling protein called IL-2. These IL-2-secreting cells are the ones that remain in the body and “remember” how to fight off the virus.
“Without the IL-2 signaling protein, you’ll generate a beautiful primary response against a virus, and you’ll eliminate the bug, but your body won’t remember how it defeated the virus,” Dr. Farrar said. “Without these memory cells, your body is defenseless against re-infections.”
Ann Davis, student research assistant in immunology and lead author of the study, said this suggests a new role for interferon: teacher.
“This is really the first demonstration of a role for interferon in teaching a T cell how to respond to viral infections,” she said.
Dr. Farrar added: “Up until now, interferon has always been appreciated for its role in inhibiting virus infections. But no one’s really paid attention to interferon and its role in regulating memory. That’s why we’re so excited about this result.”
The next step, Dr. Farrar said, is to complete the same study in mice. Early results show that mice with T cells that can’t respond to interferon are unable to protect themselves when a virus invades.
“Their immune systems have no idea how to fight the virus,” Dr. Farrar said.
Dr. Farrar said these early findings in mice may pave the way for designing more effective vaccines.
Other UT Southwestern researchers involved in the study were Hilario Ramos, student research assistant in immunology, and Dr. Laurie Davis, associate professor of internal medicine.
The National Institutes of Health supported the research.
Dr. David Farrar — http://www.utsouthwestern.edu/findfac/professional/0,2356,12163,00.html
Media Contact
More Information:
http://www.utsouthwestern.eduAll latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
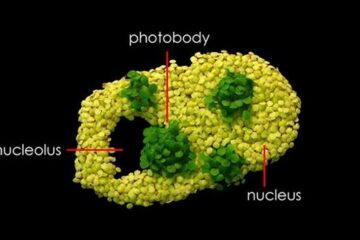
Free-forming organelles help plants adapt to climate change
Scientists uncover how plants “see” shades of light, temperature. Plants’ ability to sense light and temperature, and their ability to adapt to climate change, hinges on free-forming structures in their…