Investigational eye treatment: Corneal collagen crosslinking research study

Keratoconus is a disease of the cornea, the clear front lens of the eye (like the crystal on a watch), that occurs in the overall population at a rate of about one in 2000. It usually begins in the teens and 20's and can worsen over time. It is often discovered when vision cannot be properly corrected with glasses. Keratoconus results in thinning of the corneal tissues.
Consequently, the cornea bulges out of its smooth, clear, dome-like structure, and assumes a more conical and irregular configuration. Because of this change in shape, the cornea loses its ability to form a clear image in the eye and the patient's vision can decrease drastically. Treatments include specialty keratoconus contact lenses and corneal inlays. However, the keratoconus cornea can continue to bulge over time and some keratoconus patients ultimately may require corneal transplantation to regain vision.
Corneal collagen crosslinking (CXL) using ultraviolet light combined with riboflavin (Vitamin B2) is an investigational procedure designed to strengthen the cornea and decrease the progression of keratoconus. CXL is an investigational procedure and is not approved for use in the United States. However, here at the CLEI Center for Keratoconus, we are participating in a research study of CXL. The goal of the study is to assess the safety and efficacy of crosslinking for the treatment of keratoconus as well as corneal ectasia after LASIK. If successful, CXL may decrease progression of keratoconus and maintain the patient's vision over time.
During the crosslinking procedure, anesthesia drops are administered. The surface epithelial cells of the cornea are then removed and riboflavin drops are administered for 30 minutes. The riboflavin acts both to enhance the crosslinking effect and to protect the rest of the eye from the UV exposure.
The patient then looks at a UV emitting light for 30 minutes. At the conclusion of the procedure, a soft contact lens bandage is applied. The contact lens is left in place to improve healing for approximately 5 days and is then removed. Antibiotic and anti-inflammatory drops are used for two weeks afterwards.
Dr. Hersh, a cornea and refractive surgery specialist in Teaneck, NJ, founded the Cornea and Laser Eye Institute in 1995, and its specialty CLEI Center for Keratoconus in 2002. Dr. Hersh is also Clinical Professor of Ophthalmology and Director of Cornea and Refractive Surgery at UMDNJ-New Jersey Medical School, and Visiting Research Collaborator at Princeton University.
For more research study information please call 201-883-0505
Media Contact
More Information:
http://www.vision-institute.comAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Why getting in touch with our ‘gerbil brain’ could help machines listen better
Macquarie University researchers have debunked a 75-year-old theory about how humans determine where sounds are coming from, and it could unlock the secret to creating a next generation of more…

Attosecond core-level spectroscopy reveals real-time molecular dynamics
Chemical reactions are complex mechanisms. Many different dynamical processes are involved, affecting both the electrons and the nucleus of the present atoms. Very often the strongly coupled electron and nuclear…
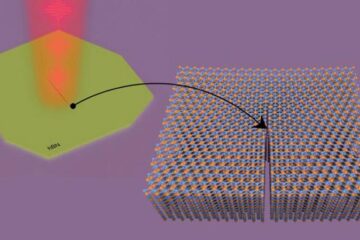
Columbia researchers “unzip” 2D materials with lasers
The new technique can modify the nanostructure of bulk and 2D crystals without a cleanroom or expensive etching equipment. In a new paper published on May 1 in the journal…





















