Using artificial intelligence to determine whether immunotherapy is working
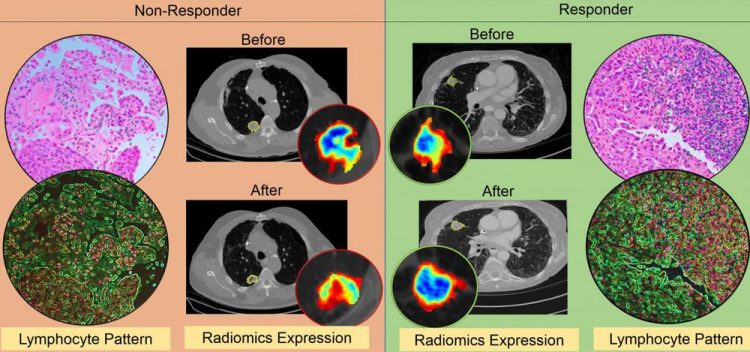
An illustration of the differences in CT radiomic patterns before and after initiation of checkpoint inhibitor therapy. Also, density of tumor infiltrating lymphocytes, on diagnostic biopsies, was found to be higher in responders as compared to non-responders. Credit: Case Western Reserve University
Scientists from the Case Western Reserve University digital imaging lab, already pioneering the use of Artificial Intelligence (AI) to predict whether chemotherapy will be successful, can now determine which lung-cancer patients will benefit from expensive immunotherapy.
And, once again, they're doing it by teaching a computer to find previously unseen changes in patterns in CT scans taken when the lung cancer is first diagnosed compared to scans taken after the first 2-3 cycles of immunotherapy treatment. And, as with previous work, those changes have been discovered both inside–and outside–the tumor, a signature of the lab's recent research.
“This is no flash in the pan–this research really seems to be reflecting something about the very biology of the disease, about which is the more aggressive phenotype, and that's information oncologists do not currently have,” said Anant Madabhushi, whose Center for Computational Imaging and Personalized Diagnostics (CCIPD) has become a global leader in the detection, diagnosis and characterization of various cancers and other diseases by meshing medical imaging, machine learning and AI.
Currently, only about 20% of all cancer patients will actually benefit from immunotherapy, a treatment that differs from chemotherapy in that it uses drugs to help your immune system fight cancer, while chemotherapy uses drugs to directly kill cancer cells, according to the National Cancer Institute.
Madabhushi said the recent work by his lab would help oncologists know which patients would actually benefit from the therapy, and who would not.
“Even though immunotherapy has changed the entire ecosystem of cancer, it also remains extremely expensive–about $200,000 per patient, per year,” Madabhushi said. “That's part of the financial toxicity that comes along with cancer and results in about 42% of all new diagnosed cancer patients losing their life savings within a year of diagnosis.”
Having a tool based on the research being done now by his lab would go a long way toward “doing a better job of matching up which patients will respond to immunotherapy instead of throwing $800,000 down the drain,” he added, referencing the four patients out of five who will not benefit, multiplied by annual estimated cost.
New research published
The new research, led by co-authors Mohammadhadi Khorrami and Prateek Prasanna, along with Madabhushi and 10 other collaborators from six different institutions (see list, below) was published this month in the journal Cancer Immunology Research.
Khorrami, a graduate student working at the CCIPD, said one of the more significant advances in the research was the ability of the computer program to note the changes in texture, volume and shape of a given lesion, not just its size.
“This is important because when a doctor decides based on CT images alone whether a patient has responded to therapy, it is often based on the size of the lesion,” Khorrami said. “We have found that textural change is a better predictor of whether the therapy is working.
“Sometimes, for example, the nodule may appear larger after therapy because of another reason, say a broken vessel inside the tumor–but the therapy is actually working. Now, we have a way of knowing that.”
Prasanna, a postdoctoral research associate in Madabhushi's lab, said the study also showed that the results were consistent across scans of patients treated at two different sites and with three different types of immunotherapy agents.
“This is a demonstration of the fundamental value of the program, that our machine-learning model could predict response in patients treated with different immune checkpoint inhibitors,” he said. “We are dealing with a fundamental biological principal.”
Prasanna said the initial study used CT scans from 50 patients to train the computer and create a mathematical algorithm to identify the changes in the lesion. He said the next step will be to test the program on cases obtained from other sites and across different immunotherapy agents. This research recently won an ASCO 2019 Conquer Cancer Foundation Merit Award.
Additionally, Madabhushi said, researchers were able show that the patterns on the CT scans which were most associated with a positive response to treatment and with overall patient survival were also later found to be closely associated with the arrangement of immune cells on the original diagnostic biopsies of those patients.
This suggests that those CT scans actually appear to capturing the immune response elicited by the tumors against the invasion of the cancer–and that the ones with the strongest immune response were showing the most significant textural change and most importantly, would best respond to the immunotherapy, he said.
Madabhushi established the CCIPD at Case Western Reserve in 2012. The lab now includes nearly 60 researchers.
Some of the lab's most recent work, in collaboration with New York University and Yale University, has used AI to predict which lung cancer patients would benefit from adjuvant chemotherapy based on tissue-slide images. That advancement was named by Prevention Magazine as one of the top 10 medical breakthroughs of 2018.
###
Other authors on the paper were: Germán Corredor, Mehdi Alilou and Kaustav Bera from Biomedical Engineering, Case Western Reserve University; Pingfu Fu from Population and Quantitative Health Sciences, Case Western Reserve University; Amit Gupta of University Hospitals Cleveland Medical Center; Pradnya Patil of Cleveland Clinic; Priya D. Velu of Weill Cornell Medicine; Rajat Thawani of Maimonides Medical Center; Michael Feldman from Perelman School of Medicine of the University of Pennsylvania; and Vamsidhar Velcheti from NYU-Langone Medical Center.
Case Western Reserve University is one of the country's leading private research institutions. Located in Cleveland, we offer a unique combination of forward-thinking educational opportunities in an inspiring cultural setting. Our leading-edge faculty engage in teaching and research in a collaborative, hands-on environment. Our nationally recognized programs include arts and sciences, dental medicine, engineering, law, management, medicine, nursing and social work. About 5,100 undergraduate and 6,200 graduate students comprise our student body. Visit case.edu to see how Case Western Reserve thinks beyond the possible.
Media Contact
More Information:
http://dx.doi.org/10.1158/2326-6066.CIR-19-0476All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

High-energy-density aqueous battery based on halogen multi-electron transfer
Traditional non-aqueous lithium-ion batteries have a high energy density, but their safety is compromised due to the flammable organic electrolytes they utilize. Aqueous batteries use water as the solvent for…

First-ever combined heart pump and pig kidney transplant
…gives new hope to patient with terminal illness. Surgeons at NYU Langone Health performed the first-ever combined mechanical heart pump and gene-edited pig kidney transplant surgery in a 54-year-old woman…

Biophysics: Testing how well biomarkers work
LMU researchers have developed a method to determine how reliably target proteins can be labeled using super-resolution fluorescence microscopy. Modern microscopy techniques make it possible to examine the inner workings…





















