Survival without lasting damage
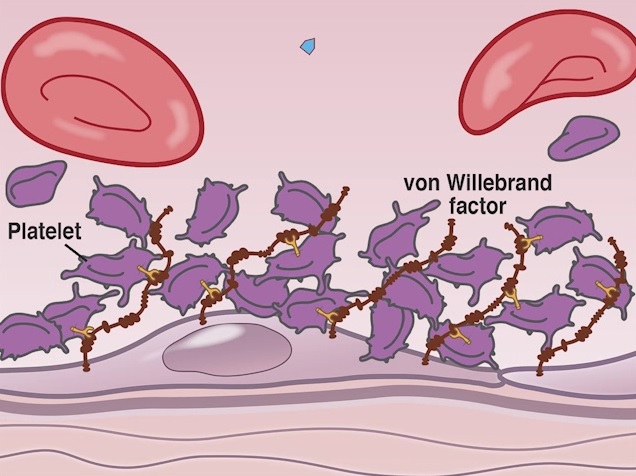
Schematic presentation of platelets (purple) which stick to the over-long Von Willebrand factor (brown). Massachusetts Medical Society
The rare and life-threatening blood disorder thrombotic thrombocytopenic purpura (TTP) mainly affects young, otherwise healthy people aged between 20 and 50. Only 2-3 people out of every million will fall ill with TTP, which forms blood clots in the small blood vessels.
The decreased blood flow damages the heart, brain and kidneys in particular and can lead to strokes and heart attacks. The disorder mainly affects women and will lead to death in over 90 percent of cases if it is not treated within a few days.
Autoimmune disorder with lasting consequences
TTP is an autoimmune disorder with antibodies against the ADAMTS13 protein enzyme. Through the acute lack of ADAMTS13, the von Willebrand factor is no longer regulated in terms of size and blood platelets spontaneously adhere to it. For this reason, the standard treatment at the moment consists of daily plasma exchange (removal of antibodies, supply of ADAMTS13) and immunosuppressive drugs.
Despite the treatment, 10-20 percent of patients die during the acute episode. More than half of patents are left with neurological damage as a result of the decreased blood flow, such as impaired concentration, attention deficit and visual problems, numbness in an arm or leg and paralysis of these. With almost half, the disorder flares up again within 1-2 years.
Rapid control of the disorder with lower rate of relapses
In a multicentre clinical study (CH, AU, IT, BE, USA) with the involvement of the Department of Hematology of the Bern University Hospital, it has now been possible to treat TTP with an anti-von Willebrand factor nanobody, which prevents the blood platelets from adhering. As a result, TTP can be forced back within a few days and the organs are protected from further decreased blood flow – which prevents at least some of the remaining damage.
75 patients were involved in the study. Together with the standard treatment, 36 patients received the new active ingredient and the 39 patients of the control group received a placebo. Bern-based haematologist Johanna Kremer Hovinga analysed all the blood samples and found that in 95 percent of patients, who received the new active ingredient, the acute phase of TTP had ended after scarcely 4 days, making this almost 40 percent faster than with the traditional treatment.
The side-effects were generally comparable, but light bleeding occurred more frequently with the new active ingredient (54% of patients in comparison with 38% with the placebo). As long as the medication was given, no patient had a relapse, although the autoimmune reaction continued to be active in at least 20 percent of patients. Another advantage: Because the new active ingredient can be injected subcutaneously, it was possible to treat patients on an outpatient basis after just a few days.
Long-term special subject at the Bern University Hospital and Bern University
The Department of Hematology at the Bern University Hospital and the University of Bern have been researching TTP and ADAMTS13 since the mid-1990s and have published extensive work in this. This study in the New England Journal of Medicine is the first major randomised patient study in the field of the rare disorder of TTP and shows a promising new treatment approach based on expanded knowledge of TTP.
Contact: Prof. Dr.med. Johanna Kremer Hovinga Strebel, senior consultant, Department of Hematology and Central Hematology Laboratory, Bern University Hospital, +41 31 632 02 65.
http://www.insel.ch/en/
http://www.nejm.org/doi/full/10.1056/NEJMoa1505533
Media Contact
All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Making diamonds at ambient pressure
Scientists develop novel liquid metal alloy system to synthesize diamond under moderate conditions. Did you know that 99% of synthetic diamonds are currently produced using high-pressure and high-temperature (HPHT) methods?[2]…

Eruption of mega-magnetic star lights up nearby galaxy
Thanks to ESA satellites, an international team including UNIGE researchers has detected a giant eruption coming from a magnetar, an extremely magnetic neutron star. While ESA’s satellite INTEGRAL was observing…
Solving the riddle of the sphingolipids in coronary artery disease
Weill Cornell Medicine investigators have uncovered a way to unleash in blood vessels the protective effects of a type of fat-related molecule known as a sphingolipid, suggesting a promising new…





















