Modeling NAFLD with human pluripotent stem cell derived immature hepatocyte like cells
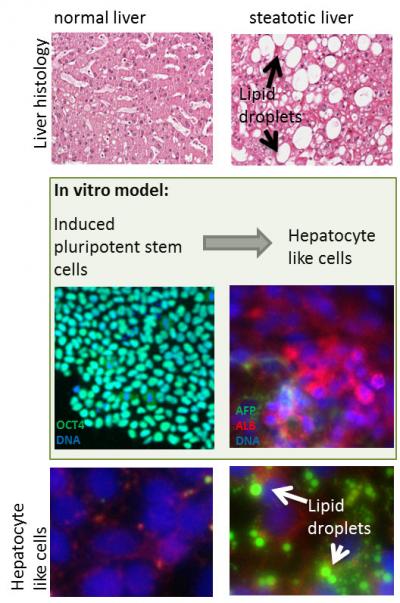
Histological section of a liver biopsy of a healthy individual (upper left) and an NAFLD patient (upper right) (1). Lipid droplets are visible as vacuoles. Induced pluripotent stem cells, which express the pluripotency marker OCT4 (middle left, green), are in vitro differentiated into hepatocyte-like cells, characterized by the expression of ALBUMIN (ALB, middle right, red) and alpha-fetoprotein (AFP, middle green right). Unstimulated in vitro derived hepatocyte-like cells do not incorporate lipid droplets (lower left) while they develop massive lipid droplets after stimulation with oleic acid (lower right, green). Credit: Graffmann N et al.
Researchers from the Institute for Stem Cell Research and Regenerative Medicine at the University Clinic of Düsseldorf have established an in vitro model system for investigating nonalcoholic fatty liver disease (NAFLD). The study led by Prof. James Adjaye has now been published in the journal Stem Cells and Development.
Nonalcoholic fatty liver disease (NAFLD), also called steatosis, is a dramatically under-estimated liver disease, with increasing incidences throughout the world. It is frequently associated with obesity and type-2 diabetes. Approximately one third of the general population in Western countries are affected, often without even having symptoms.
It is a result of a high caloric diet in combination with a lack of exercise, where the liver starts incorporating fat as lipid droplets. Initially, this is a benign state, which can, however, develop into NASH /steatohepatitis, an inflammatory disease of the liver. Then many patients develop fibrosis, cirrhosis or even liver cancer. However, in many cases patients die of heart failure before they develop severe liver damage.
A major obstacle for NAFLD research was, up to now, that biopsies of patients and healthy individuals were required. The Düsseldorf researchers elegantly solved this problem by reprogramming skin cells into so called induced pluripotent stem cells which they differentiated into hepatocyte like cells. “Although our hepatocyte-like cells are not fully mature, they are already an excellent model system for the analysis of such a complex disease”, explains Dr. Nina Graffmann, first author of the study.
The researchers recapitulated important steps of the disease in vitro. For example they demonstrated up-regulation of PLIN2, a protein that covers lipid droplets. Mice without PLIN2 do not become obese, even when overfed with a high fat diet. Also the key role of PPARα, a transcription factor involved in controlling glucose and lipid metabolism, was reproduced in the in vitro system.
“In our system, we can efficiently induce lipid storage in hepatocyte-like cells and manipulate associated proteins or microRNAs by adding various factors into the culture. Thus, our in vitro model offers the opportunity to analyse drugs which might reduce the stored fat in hepatocytes” says Dr. Graffmann.
The team now expands the model using induced pluripotent stem cells derived from NAFLD patients, hoping to discover differences which might explain the course of the disease.
“Using as reference the data and biomarkers obtained from our initial analyses on patient liver biopsies and matching serum samples (1), we hope to better understand the etiology of NAFLD and the development of NASH at the level of the individual, with the ultimate aim of developing targeted therapy options,” states Professor James Adjaye, senior author of the current study.
###
Publication: Graffmann N, Ring S, Kawala MA, Wruck W, Ncube A, Trompeter HI, et al. Modelling NAFLD with human pluripotent stem cell derived immature hepatocyte like cells reveals activation of PLIN2 and confirms regulatory functions of PPARalpha. Stem Cells and Development. 2016.
Media Contact
All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Superradiant atoms could push the boundaries of how precisely time can be measured
Superradiant atoms can help us measure time more precisely than ever. In a new study, researchers from the University of Copenhagen present a new method for measuring the time interval,…

Ion thermoelectric conversion devices for near room temperature
The electrode sheet of the thermoelectric device consists of ionic hydrogel, which is sandwiched between the electrodes to form, and the Prussian blue on the electrode undergoes a redox reaction…

Zap Energy achieves 37-million-degree temperatures in a compact device
New publication reports record electron temperatures for a small-scale, sheared-flow-stabilized Z-pinch fusion device. In the nine decades since humans first produced fusion reactions, only a few fusion technologies have demonstrated…





















