Vitamin D: Total but Not Dietary Alone Prevents Colorectal Cancer

Studies of the geographic variation of colon and rectal (colorectal) cancer mortality rates in the U.S. have long indicated that they are primariliy linked to solar ultraviolet-B (UVB) radiation: the more UVB in summer, the lower the mortality rate.
The hypothesis to explain this result is that UVB radiation produces vitamin D in the skin, and vitamin D acts to reduce the risk of colorectal and over a dozen other types of cancer. One major study found that intake of 150 IU/day of vitamin D was associated with a reduction by half in incidence of colon cancer, a result that was statistically significant. However, some studies that have investigated the link between dietary sources of vitamin D and colorectal cancer have found a smaller degree of risk reduction comparing the highest versus lowest levels of dietary vitamin D.
In a review of the literature published in the current issue of Nutrition and Cancer, Drs. William Grant and Cedric Garland report that the reason for the sometimes weak link between dietary sources of vitamin D and colorectal cancer incidence or mortality rates is that dietary sources often cannot supply enough vitamin D to be effective in quantities ordinarily consumed. In most such studies, the highest quartile or quintile of those studied consumed over 150-370 I.U./day from dietary sources. That was sufficient in some cases to provide a 10-50% reduction in colorectal cancer risk, but not always at a statistically significant level. However, studies that considered vitamin D intake from both diet and supplements for which the highest levels were over 500 I.U./day found 30-60% risk reduction for the highest versus lowest levels, and the results were uniformly tatistically significant.
These results, then, help explain the geographic variation of colorectal and other cancer mortality rates in the U.S. Colon cancer mortalty rates for males in the period 1970-94 were about 25 deaths/100,000/year (d/hk/yr) for males and 18 d/hk/yr for females in northeastern states but only 15 d/hk/yr for males and 12 d/hk/yr for females in southwestern states.
These mortality rates are inversely correlated with July average irradiances of solar UVB radiation, which are higest in the southwest, lowest in the northeast taking into further consideration that urbanites have reduced UVB exposure compared to rural residents. These results are consistent with those living in the southwestern states having an effective annual average vitamin D production of several hundred I.U./day more than those living in the northeastern states. In addition, these results provide further support for the idea that most Americans obtain most of their vitamin D from solar UVB radiation and not diet.
As reported earlier, Dr. Grant estimates that over 20,000 Americans die prematurely from over a dozen types of cancer annually due to insufficient UVB/vitamin D [Grant, 2002]. This number is much higher than the approximately 9,000 who die annually from melanoma in the U.S. or approximately 2,000 from non-melanoma skin cancer.
It should be noted that while UV radiation, especially UVA, plays a role in both melanoma and non-melanoma skin cancer, a number of other factors also play important roles, such as skin pigmentation, severe sunburning, a high-fat, high-protein, low-fruit and vegetable diet, and alcohol consumption [Millen et al., 2004] and, at least for non-melanoma skin cancer, cigarette smoking. Together, these factors explain about half of melanoma and non-melanoma death rates.
Most people should be able to obtain adequate levels of vitamin D from modest daily exposures to mid-day summer sun in the southwest up through Wyoming and the southeastern states, with longer exposures required in other locations.
When solar UVB levels are not adequate, such as during the winter in most areas, vitamin D3 supplements or artificial UV lamps that mimic the solar UVA and UVB spectrum may provide convenient alternate sources of vitamin D.
Grant WB, Garland CF. A critical review of studies on vitamin D in relation to colorectal cancer. Nutrition and Cancer, 2004;48:115-23.
William B. Grant, Ph.D.
SUNARC
2107 Van Ness Avenue, Suite 403B
San Francisco, CA 94109
Cedric F. Garland, Dr.P.H., F.A.C.E.
Department of Family and Preventive Medicine, 0631C
School of Medicine
University of California, San Diego
9500 Gilman Drive
La Jolla, California 92093-0631, USA
Media Contact
More Information:
http://www.sunarc.orgAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
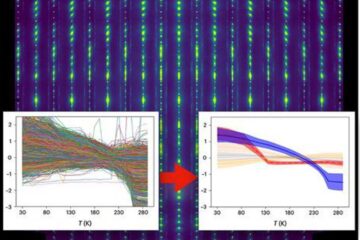
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















