Fighting fire with fire? Vaccine based on chimp virus shows promise against HIV

In a new study in mice, a modified form of an innocuous chimpanzee virus has shown marked potency as a protective vaccine against HIV, itself believed to have crossed into the human population from chimpanzees sometime in the 1930s. The study, led by researchers at The Wistar Institute, appears in the February issue of the Journal of Immunology.
“Our results show this new vaccine is capable of inducing the kind of powerful immune response that we and others believe will be critical for controlling HIV infection,” says Hildegund C.J. Ertl, M.D., professor and immunology program leader at The Wistar Institute, and senior author on the new study.
Given the history of HIV, Ertl emphasize the lengths to which she and her colleagues have gone to ensure that the new vaccine is completely safe. To eliminate the possibility of any contaminant – an HIV-like stowaway, for example – the vaccine is derived in the laboratory from a set of genetic instructions. Importantly, too, the genes that would be needed by the viral vaccine to replicate are deleted from those instructions.
The vaccine is based on a chimpanzee adenovirus. In chimpanzees and humans, adenoviruses are a common cause of respiratory-tract infections. Immunologists have understood for some time that human adenoviruses can be retooled in the laboratory to serve as the basis for vaccines against an array of viral diseases. They easily enter human cells and stimulate a vigorous, long-lasting immune response. A number of vaccines based on human adenoviruses, including some against HIV, are now in development.
An unaddressed concern with these vaccines, however, is the question of pre-existing immunity. Adenoviruses are nearly ubiquitous among humans, so much so that more than 45 percent of the population has neutralizing antibodies circulating in the blood able to impair any vaccine based on a common human adenovirus. But the new chimpanzee adenovirus vaccine possesses the immunological strengths of a human adenovirus vaccine without the drawback of pre-existing immunity in its target population.
Because HIV infects only humans and chimpanzees, the current study used a sophisticated mouse model to test the new vaccine. For this model, the researchers first incorporated an internal HIV protein known as gag into the modified chimpanzee adenovirus vaccine. They also engineered a matching vaccine that incorporated gag into the human adenovirus. They then used a variant of the vaccinia virus, which can infect mice, that included the gag protein. For comparison, some mice were exposed to the human adenovirus, so that they would demonstrate the pre-existing immunity to the virus seen in many humans.
After vaccination with the chimpanzee adenovirus vaccine, the mice mounted a powerful T-cell-based immune response and were able to fight off experimental infection by the vaccinia virus containing gag, the HIV protein. The mice pre-exposed to the human adenovirus and vaccinated with the human adenovirus vaccine, however, demonstrated significantly weaker immune responses to the vaccinia virus.
“It’s hard to say that because the vaccine works well in a mouse model, it will protect humans from HIV infection,” Ertl cautions. “But we do know that the kind of immune response we saw in mice can protect non-human primates infected with SIV from developing disease.” SIV, or simian immunodeficiency virus, is the chimpanzee counterpart to HIV, or human immunodeficiency virus.
In addition to moving forward with testing of the chimpanzee adenovirus vaccine against HIV, Ertl and her colleagues are developing similar vaccines against rabies, smallpox, and a number of other viruses.
Julie C. Fitzgerald, a graduate student in senior author Ertl’s laboratory, is lead author on the Journal of Immunology study. The other Wistar-based authors are Zhi Q. Xiang, Anthony P. Wlazlo, and Wynetta Giles-Davis. Arturo Reyes-Sandoval is affiliated with Wistar and the Instituto Politecnico Nacional in Mexico City. George N. Pavlakis is with the National Cancer Institute. Guang-Ping Gao and James M. Wilson are with the University of Pennsylvania. The techniques used to create the vaccine were developed under the guidance of Wilson and his colleagues.
Funding for the research was provided by the National Institutes of Health, the W.W. Smith Foundation, and Genovo. Wilson owns equity in Targeted Genetics, formerly Genovo.
The Wistar Institute is an independent nonprofit biomedical research institution dedicated to discovering the causes and cures for major diseases, including cancer, cardiovascular disease, autoimmune disorders, and infectious diseases. Founded in 1892 as the first institution of its kind in the nation, The Wistar Institute today is a National Cancer Institute-designated Cancer Center – one of only eight focused on basic research. Discoveries at Wistar have led to the development of vaccines for such diseases as rabies and rubella, the identification of genes associated with breast, lung, and prostate cancer, and the development of monoclonal antibodies and other significant research technologies and tools.
Media Contact
More Information:
http://www.wistar.upenn.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
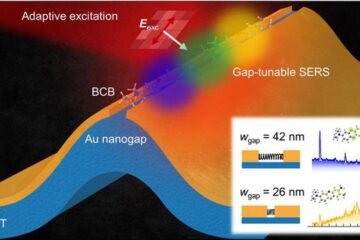
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















