A novel method to prevent hemorrhagic complications of thrombolytic therapy of blood clots is discovered

Many safe therapy forms, however, are often associated with hazards, and therefore indications for therapy must be weighed on an individual basis. In stroke thrombolysis, it is the risk of perithrombolytic hemorrhage formation and expansive brain edema that are most feared complications, and may preclude from administering the therapy. Even after proper precautions, perithrombolytic hemorrhages occur in 6 to 10 % of treated patients. Therefore, experimental research is needed to clarify the mechanisms leading to these complications.
The now reported study led by Dr. Perttu J. Lindsberg from the Helsinki University Central Hospital investigated thrombolytics-related brain hemorrhage formation in an experimental stroke model in rats. It found that, in addition to the clot lysing effect, the drug used for this purpose, alteplase (recombinant tissue plasminogen activator) also possesses proinflammatory properties and activates and degranulates mast cells, a kind of tissue-based immune cell. On degranulation, mast cells release potent enzymes that cleave proteins (eg, chymase, tryptase, and metalloproteases) in the vessel wall. The result is increased vascular permeability, which can lead to hazardous brain edema and potentially to frank brain hemorrhage formation. A pharmacological mast cell stabilizer, cromoglycate, was administered before alteplase, and it reduced these detrimental effects significantly and led to improved neurological outcome and reduced mortality.
The amount of brain hemorrhage was reduced by 97% at 3 hours, by 76% at 6 hours, and by 96% after 24 hours of follow-up. Ischemic brain edema was reduced by 80% at 3 hours, by 55% at 6 hours and by 85% after 24 hours of follow-up. The mortality in control group was 29%, 64% in alteplase group, and 0% in a group treated with a combination of alteplase and cromoglycate. kromoglikaatti+alteplaasiryhmässä 0%). Furthermore, genetically engineered animals were used which lacked mast cells, and they showed minimal brain edema and alteplase-related hemorrhage formation. They also had improved neurological outcome and mortality compared with wild-type littermates. In addition to proteolytic enzymes, mast cells release vasodilators such as histamine as well as heparin (s.c. “blood thinning” anticoagulant drug), which may locally prevent blood coagulation, predispose to bleeding and edema formation and ultimately lead to hazardous expansion of hemorrhagic and edematous brain events. The intracranial space is tight and does not allow expansion of its tissue content without harmful and potentially fatal consequences.
This study revealed a novel proinflammatory cellular mechanism related to an every-day dilemma in routine patient care that may provide a novel pharmacological target if confirmed in the clinical setting. At best, mast cell stabilization could eventually be applied as an adjuvant to thrombolysis.
Media Contact
More Information:
http://www.helsinki.fiAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
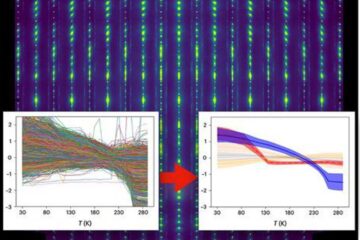
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















