Aspirin reduces esophageal-cancer risk in people with most-aggressive form of Barrett's esophagus

Researchers at Fred Hutchinson Cancer Research Center have found that people with the most-aggressive form of Barrett’s esophagus, a precancerous condition that can lead to esophageal cancer, may benefit the most from preventive therapy with aspirin, ibuprofen and other nonsteroidal anti-inflammatory drugs, or NSAIDs. The researchers also identified a cluster of four known cancer biomarkers, or genetic abnormalities, in people with Barrett’s that significantly increases their risk of developing esophageal cancer.
These findings, by lead authors Patricia C. Galipeau and Xiaohong Li, senior author Brian J. Reid, M.D., Ph.D., and colleagues in the Hutchinson Center-based Seattle Barrett’s Esophagus Program, will be published in the Feb. 27 issue of PLoS Medicine, a freely available online journal. Researchers from Virginia Mason Medical Center, Harvard Medical School and The Wistar Institute collaborated on the study, which was funded by the National Institutes of Health and the Hutchinson Center.
The researchers found that those with three or more of the cancer biomarkers upon enrollment in the study who also used aspirin or other NSAIDs had a 30 percent risk of esophageal cancer after 10 years, while those with the same biomarkers who did not use NSAIDs had a 79 percent risk of developing cancer within a decade of joining the study.
“This is the first prospective, longitudinal study in patients with Barrett’s esophagus – or any other pre-malignant condition, for that matter – to link somatic genetic biomarkers for cancer-risk prediction with candidate interventions such as NSAIDs to prevent cancer,” said Galipeau, a research technician in Reid’s laboratory, which is based in the Hutchinson Center’s Human Biology Division.
The researchers also found that Barrett’s patients whose esophageal tissue had no such genetic abnormalities, or biomarkers, upon joining the study had a 12 percent risk of developing esophageal cancer after 10 years, whereas those with three or more of the abnormalities at baseline had a nearly 80 percent risk of developing such cancer within a decade.
“Several studies have suggested that individual genetic abnormalities may identify Barrett’s patients who are at increased risk of progression toward esophageal cancer, but this is the first study to evaluate the combined contribution of genetic abnormalities for esophageal cancer-risk prediction,” said Reid, director of the Seattle Barrett’s Esophagus Program.
The study followed 243 people with Barrett’s esophagus for 10 years (189 male, 54 female, mean age 62 upon joining the study). The participants were interviewed about their medical history, diet and medication use and were closely monitored for signs of disease progression through regular endoscopies and tissue biopsies.
Their Barrett’s-related esophageal tissue was evaluated at the initial study visit for a variety of known cancer biomarkers, but the genetic abnormalities that were most strongly predictive of progression toward cancer were:
Loss of heterozygosity (LOH) at 9p and 17p – loss on the short arms of chromosomes 17 and 9. Such chromosomal abnormalities inactivate tumor-suppressor genes that are critical for controlling cell growth.
DNA content abnormalities (aneuploidy and tetraploidy) – the accumulation of cells with grossly abnormal amounts of DNA, which indicates substantial genetic damage and heralds advanced progression toward cancer.
Ultimately, the researchers hope, these biomarkers one day could be used in a clinical setting to identify which Barrett’s patients are most likely to develop esophageal cancer and therefore benefit from aggressive cancer surveillance via endoscopy and chemoprevention with aspirin and other NSAIDs. Galipeau and colleagues are in the process of developing such a standardized, biomarker-based screening test. The test would evaluate DNA from esophageal-tissue biopsies, but significantly fewer tissue samples would need to be collected as compared to current endoscopic-surveillance methods.
“Once such a test is available, it could be a major factor in guiding the development of clinical trials to identify high-risk patients and definitively determine the value of NSAIDs in preventing the progression of Barrett’s esophagus toward cancer,” Reid said.
It is hypothesized that aspirin and other NSAIDs may fight cancer by reducing chronic inflammation, which is a driving force behind the development of many cancers and other diseases. Specifically, NSAIDs have been shown to inhibit the production of the cyclooxygenase-2 (COX-2) enzyme. Disruption of this pathway slows the growth of abnormal cells and facilitates the normal process of programmed cell death, or apoptosis, both of which can thwart cancer development. NSAIDs are also believed to decrease proliferation of cells and decrease the growth of blood vessels that supply blood to tumors, Reid said.
The annual incidence of esophageal cancer among Barrett’s esophagus patients is about 1 percent – most patients never get the cancer. However, the outlook is grim if the cancer is not diagnosed early, with an overall survival rate of only 13.7 percent. For this reason, Barrett’s patients must undergo frequent endoscopic surveillance.
“Many Barrett’s patients are subjected to overdiagnosis of risk and overtreatment,” Reid said. “These findings ultimately may help us identify high-risk patients who truly require frequent surveillance and low-risk patients who need no or less-frequent surveillance. For example, low-risk patients with no biomarker abnormalities at baseline had a zero percent cumulative risk of developing esophageal cancer for nearly eight years,” he said. “These findings also may help us determine which Barrett’s patients may benefit most from a very cost-effective, noninvasive therapy in the form of aspirin or NSAIDs.”
Currently, the recommended endoscopic screening frequency for Barrett’s esophagus ranges from once every three to six months to once every two to three years, depending on the amount of affected tissue and the degree of dysplasia, or cellular abnormality, detected upon examining a tissue sample under a microscope. While cellular dysplasia is the most common method for determining the severity, or grade, of Barrett’s, several recent studies have found that the technique is not truly predictive of cancer risk. Longitudinal studies of high-risk Barrett’s patients (as determined by degree of cellular dysplasia) have found cancer-incidence rates ranging from 8 percent to 59 percent. “Clearly we need a new, more consistent and reliable way to predict risk that doesn’t rely on the subjective interpretation of a pathologist,” said Reid, also a professor of gastroenterology and medicine and an adjunct professor of genome sciences at the University of Washington School of Medicine.
Media Contact
All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
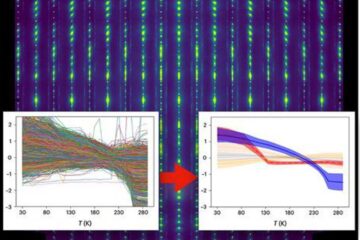
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















