Lung cancer: New techniques improve radiation therapy

However, so far only 10 to 15 percent of lung cancer patients can be cured permanently. More than half of the patients with a small-cell lung carcinoma and about 65 percent of the patients with a non-small-cell lung carcinoma receive radiation treatment in the course of their illness.
The precision of a three-dimensional radiation planning is, however, limited by nature in the case of lung cancer: During breathing, the tumors shift by a few centimeters. As a consequence, the target area “moves” and can be missed if the radiation limits have been chosen too narrowly. Then the tumor cells will keep growing. But if the radiotherapist chooses the limits of the radiation field too generously, more side effects in the healthy lung are to be expected.
Image guided radiotherapy.
The image guided radiotherapy (IGRT) offers a solution to this dilemma, as experts report at the ESTRO congress in Leipzig. Novel linear accelerators that are equipped with a special x-ray device depict the tumor immediately before the radiation treatment. This allows capturing “moving” target areas. The device registers whether the planned situation matches the real situation. If this is not the case, the computer calculates the deviation, and the radiation table is shifted accordingly.
Respiration-Adapted Radiotherapy.
The respiration-adapted radiotherapy is also promising. With this method, the radiation is activated and deactivated with the breathing. In this way, the rays always hit the tumor at the same position. In some cases, the patients are also asked to hold their breath or to breathe in a certain rhythm, which requires training the patients accordingly at the beginning of the treatment. If the anatomical shifts can be purposefully controlled, they can also be purposefully compensated for. This method is also systematically studied at the moment. Here, physicians and physicists mainly calculate how the radiation volume can be decreased by this technique.
Stereotactic radiotherapy takes the place of the scalpel.
Stereotactic radiation, which requires a lot of effort and is so far mostly used for brain tumors, is now also tested by radiotherapists on small tumors of the body stem in especially radiosensitive environments. The exact three-dimensional coordinates of the target area are determined with computer tomograms and a special planning system. To enable a precise transmission of the planned radiation data, the body of the patient is fixated with a frame during the treatment. Under computer-tomographic guidance, markings in this frame are used to direct the radiation precisely at the tumor. In most cases, this is achieved by having the radiation hit the target location from many different directions and at precisely calculated angles.
A team led by Frank Zimmermann from the Klinikum rechts der Isar in Munich presents a study with 68 patients in Leipzig, whose small lung tumors could not be operated on for general health reasons. In 3 to 5 sessions, a high radiation dose was in each case delivered by stereotactic methods. In the so far three-year follow-up period, the tumor resumed its growth in only four patients (6 percent). No serious adverse effects were observed.
Media Contact
More Information:
http://www.estro.beAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
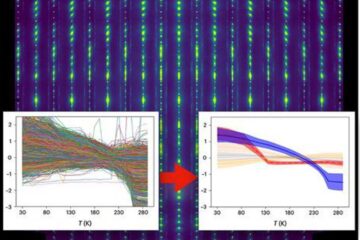
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















