Drug that battles resistance to leukemia pill Gleevec 'extremely effective' against cancer

An experimental therapy that battles drug resistance in Chronic Myeloid Leukemia (CML) has proved “extremely effective” in fighting cancer, giving patients for whom all conventional therapies have failed another option, researchers at UCLA's Jonsson Cancer Center reported.
The Bristol-Myers Squibb therapy, Sprycel (dasatinib), treats CML that has mutated and becomes resistant to the leukemia pill Gleevec, said Dr. Charles Sawyers, a professor of hematology/oncology, a Jonsson Cancer Center researcher and lead author of the study, published in the June 15, 2006 issue of the peer-reviewed New England Journal of Medicine.
The results are from a Phase I study of Sprycel. The early results were so favorable that several Phase II studies were launched last year and are almost completed. Because these trials have moved so quickly and because more positive results are anticipated, an advisory panel for the U.S. Food & Drug Administration on June 2 recommended that the agency approve the drug, which could happen before the end of the month, Sawyers said. Like Gleevec, Sprycel also is taken in pill form.
Sawyers characterized the Phase I study results as remarkable, saying the first human trial confirmed the pre-clinical laboratory work and scientific discovery done at UCLA's Jonsson Cancer Center, where the mechanisms and mutations behind Gleevec resistance were uncovered. The Phase I study was done jointly with MD Anderson Cancer Center.
“This shows that if you have a precise molecular understanding of a drug target you can very quickly decipher the reasons for response and failure to therapy and quickly come up with backup treatment strategies,” said Sawyers, a Howard Hughes Medical Institute investigator. “Gleevec remains a spectacular step forward in the field of targeted therapy. However, some patients develop resistance to the drug after several years of therapy. These patients now have another effective option in this drug.”
Drug development often can take decades. However, it has been just five years since Gleevec was approved. In that time, UCLA scientists were able to discover how the CML in some patients mutated and became resistant to Gleevec and test an existing compound on laboratory models and then in patients with great success.
Resistance in CML patients is associated with mutations in the Bcr-Abl gene that interfere with the drug's mechanism of action. Sprycel blocks 14 of 15 documented CML mutations known to lead to resistance, Sawyers said. It's about 300 times more potent than Gleevec as well.
Over five years, about 20 percent of patients become resistant to Gleevec, Sawyers said. One of the reasons Sprycel works so well to combat that resistance is that it binds to the mutant proteins in a different way than Gleevec, and it also inhibits several other tyrosine kinases believed to play roles in cancer growth, Sawyers said.
“The main message is that this drug is extremely effective in CML patients who have failed all standard therapy including Gleevec,” Sawyers said. “The basic science findings all panned out. What we predicted based on laboratory studies proved true in human trials. While there was some concern that this drug might be more toxic because it is more potent, we are delighted to find that it is very well tolerated.”
The UCLA Phase I study enrolled 84 patients – 40 with chronic phase CML, 11 with accelerated phase CML, a more serious form of the disease, and 23 whose CML was in blast crisis, the last and most serious phase of CML. Additionally, 10 patients with acute lymphoblastic leukemia (ALL) were enrolled because they tested positive for the Philadelphia chromosome, the genetic abnormality that characterizes most cases of CML and the primary mutation targeted by the drug.
A major cytogenetic response – a substantial reduction in cells containing the Philadelphia chromosome in the bone marrow – was found in 45 percent of chronic phase patients, Sawyers said. In the patients with accelerated and blast phase CML and in patients with ALL, a major cytogenetic response was reported in 43 percent of patients. The responses have lasted for up to two years in some cases and although the study is complete, a number of patients continue to take the drug and are still being monitored.
Sawyers said it's possible that Gleevec and Sprycel might be used together in patients with CML as a very effective one-two punch to fight cancer and battle drug resistance.
Lakewood resident Kevin Williams, 41, married and a father of two, was diagnosed with CML in June of 2000. He was put on interferon, the standard treatment for CML at that time. The side effects were brutal . Williams felt as if he had a bad flu all the time. He lost weight and was constantly tired. When it became clear that the interferon was not working, Williams' UCLA oncologist prescribed Gleevec, which had just been approved by the FDA.
After about 10 months on Gleevec, Williams and his oncologists noticed that he was becoming resistant to the drug. His white blood cell count was more difficult to maintain and Williams had to take more and more Gleevec to achieve a stable response. And he was showing no cytogenetic response at all. The mutated cells in his bone marrow that were causing his CML were not decreasing in number. In June 2005, Williams enrolled in a Jonsson Cancer Center study of Sprycel. A bone marrow test in February surprised Williams and his oncologists – there was absolutely no evidence in his marrow of the mutated cells. Williams was 100 percent negative for cancer just nine months after he started taking Sprycel.
“I feel like this drug has given me my life back again,” said Williams, a computer programmer. “I can now do all the things I used to do before. I feel great.”
Williams has returned to his active life, going snow skiing and road racing his motorcycle. He also spends quality time with his wife, Teresa, and his daughter, Kerri, 13, and son, Brian, 7.
Media Contact
More Information:
http://www.mednet.ucla.eduAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

Making diamonds at ambient pressure
Scientists develop novel liquid metal alloy system to synthesize diamond under moderate conditions. Did you know that 99% of synthetic diamonds are currently produced using high-pressure and high-temperature (HPHT) methods?[2]…

Eruption of mega-magnetic star lights up nearby galaxy
Thanks to ESA satellites, an international team including UNIGE researchers has detected a giant eruption coming from a magnetar, an extremely magnetic neutron star. While ESA’s satellite INTEGRAL was observing…
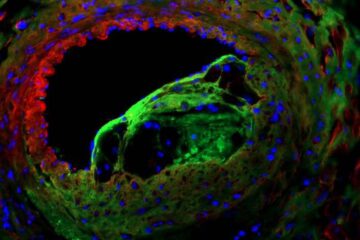
Solving the riddle of the sphingolipids in coronary artery disease
Weill Cornell Medicine investigators have uncovered a way to unleash in blood vessels the protective effects of a type of fat-related molecule known as a sphingolipid, suggesting a promising new…





















