Percutaneous aortic valve replacement

Percutaneous aortic valve replacement is becoming a reality and brings new hope for a number of patients who cannot currently be treated with traditional surgical techniques.
Whereas surgical valve replacement concerns about 200,000 patients worldwide every year, it is estimated that between 1/3 (Iung et al, Euro Heart Survey, 2003) and 2/3 (Rambas Pai, USC AHA 2004) of patients do not receive surgery due to either excessive risk factors and comorbidities or patient refusal due to fear of lifestyle changes following heavy surgery in elderly patients. The size of this untreated cohort is expected to increase, reflecting the aging population. However, without replacing the valve, the disease is associated with a very high mortality rate (50 to 60% at one year) beyond the onset of symptoms. The goal of the percutaneous valve is to bring a less invasive therapeutic solution for these patients.
The Cribier-Edwards Percutaneous valve (Edwards Lifesciences, Irvine, Cal, USA) is a bioprosthesis made of three leaflets of equine pericardium sutured to a balloon expandable stainless steel stent. After balloon predilatation of the native valve, this bioprosthesis is crimped over a balloon catheter, and advanced over a stiff guidewire through the vessels (either from the femoral vein –antegrade/transseptal approach- or the femoral artery –retrograde approach-) up to the diseased fibro-calcific native aortic valve, using regular cardiac catheterization techniques. The bioprosthesis is then released by balloon inflation at mid-part of the native valve. In our institution, the technique is performed under local anesthesia and light sedation.
In our experience, the procedure (which first case was performed in April 2002) remains under investigation and implantations are strictly restricted to compassionate cases in patients who have been formally declined by two cardiac surgeons due to severe associated comorbidities. We have enrolled 40 patients to date in two single centre feasibility studies (the I-REVIVE and the RECAST studies). Three patients have now reached two years of follow-up. The valve performance has been excellent and there has not been a single case of valve failure when the valve was successfully placed (80% of the cases). High mortality during follow-up has been related to non valvular causes, mainly the evolution of life-threatening comorbidities.
Challenges remain as the procedure is complex when performed via the antegrade/transseptal route, whereas the less demanding retrograde route has been frequently associated with failures in crossing the native valve. Also, paravalvular leaks can occur (moderate to severe in 25%), which is undesirable despite not being a clinical issue. One reason for the leak has been to have a single valve size (23mm in diameter), too small for some patients.
Two most recent developments relate to a custom retrograde delivery system, as well as a larger 26mm size valve. Dr John Webb (Vancouver, Canada) is the only physician approved yet for investigating these new iterations. He has successfully performed a number of cases using the custom retrograde delivery system and the 26mm valve. The retrograde route is much simpler and can be performed in about one hour. The rate and severity of paravalvular leak has dramatically decreased with the use of the 26mm valve.
Two multicentre studies have just begun enrollment in Europe (REVIVE trial) and the US (REVIVAL trial) that will help to determine the future of this revolutionary and promising interventional cardiology procedure.
Media Contact
More Information:
http://www.escardio.orgAll latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
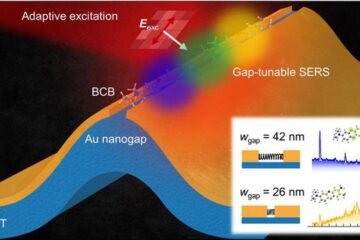
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















