ACP guidelines to treat obesity cover diet, exercise, drugs and surgery

New guidelines for management of obesity from the American College of Physicians recommend diet and exercise for everyone and drugs and surgery only for obese patients who are not able to achieve weight-loss goals with diet and exercise alone. The guidelines, “Pharmacologic and Surgical Management of Obesity in Primary Care: A Clinical Practice Guideline from the American College of Physicians,” were published in the April 5, 2005, issue of Annals of Internal Medicine.
People with a body mass index (BMI) over 30 might consider drug therapy after an appropriate trial of diet and exercise has failed. Surgery is for those with a BMI over 40 who also have obesity-related health problems such as high blood pressure, diabetes, or sleep apnea, ACP guidelines say.
People with a body mass index from 25-29.9 are considered overweight. Those with BMI from 30-39.9 are considered obese; people with a BMI over 40 are considered morbidly (or extremely) obese. BMI is a measure of height and weight. ACP’s new guidelines apply to patients with BMI’s of 30 and over.
“BMI should be considered another vital sign,” says Vincenza Snow, MD, director of clinical programs at ACP. “Patients should know their BMIs like they know their age, blood pressure and cholesterol numbers, and doctors should track their patients’ BMIs like they follow blood pressure.”
Weight-Loss Drugs
ACP identifies six drugs that according to valid clinical studies aid weight loss: sibutramine, orlistat, phentermine, diethylproprion, and fluxotine. When patients and clinicians are making decisions about use of these drugs, ACP recommends frank discussions about potential side effects and lack of long-term efficacy and safety data. (Most weight-loss drugs have no studies beyond one year.) Further, the average weight loss at one year is small to moderate, ACP says, and there are no data on whether weight loss is maintained after drug therapy is discontinued.
“Even with weight-loss drugs and even after surgery, patients must change lifestyles, eat properly and exercise,” says Snow. “There’s no magic bullet.”
Bariatric Surgery
ACP guidelines discuss several types of obesity (bariatric) surgical procedures and cautions that none have randomized, controlled trials comparing surgery with non-surgical control groups. Furthermore, all have possible side effects, ranging from surgical complications to gall bladder disease and digestion difficulties. The ACP guidelines estimate that the death rate from bariatric surgery, including in-hospital and deaths within 30 days of discharge, ranges from 0.3 in a hundred to as high as 1.9 per 100 surgeries.
ACP says that existing evidence shows a technical ’learning curve’ in bariatric surgical techniques and suggests that doctors and patients considering obesity surgery seek highly experienced surgeons and surgical centers whenever feasible.
“There are differences among the surgeries, so patients need to understand the risks of complications from surgery as well as complications further down the road, such as gall bladder disease and sometimes re-operation,” said Snow.
ACP based its guidelines on an evidence report and background papers funded by the Agency for Healthcare Research and Quality. The guidelines were developed by ACP’s Clinical Efficacy Assessment Subcommittee and were passed by the ACP Board of Regents in October 2004.
Media Contact
All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
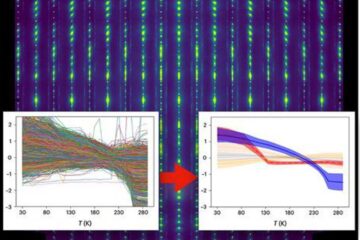
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















