New autism definition may decrease diagnosis by one-third, Columbia University finds

The guidelines, released in May 2013 and the first major update to psychiatric diagnosis criteria in almost two decades, may leave thousands of developmentally delayed children each year without the ASD diagnosis they need to qualify for social services, medical benefits and educational support.
A team led by Kristine M. Kulage, MA, MPH, director of the Office of Scholarship and Research Development at Columbia Nursing, conducted a systematic literature review and meta-analysis to determine the effect of changes to the Diagnostic and Statistical Manual of Mental Disorders (DSM), the APA's classification tool for psychiatric conditions, on diagnosis of individuals with ASD. The study found a statistically significant decrease in ASD diagnosis of 31 percent using the new manual, DSM-5, compared with the number of cases of ASD that would have been identified under the previous version of the manual, DSM-IV-TR.
“This study raises a concern that a medical provider diagnosing a child under the new guidelines won't find the child to be on the autism spectrum, when the same child under the old criteria might have been diagnosed with ASD,” says Kulage.
The old manual, DSM-IV-TR, included three distinct subgroups under the broad definition of ASD: autistic disorder (AD), Asperger's disorder, and pervasive development disorder-not otherwise specified (PDD-NOS). The revised manual, DSM-5, eliminates these subgroups, instead establishing a more limited range of criteria for a diagnosis of ASD that is designed to encompass individuals who previously would have fallen into one of the subgroups. The DSM-5 also added a new category called social communication disorder (SCD) to diagnose individuals who have verbal and nonverbal communication impairments but lack other attributes associated with autism. Some individuals diagnosed with PDD-NOS under the old manual would be identified as individuals with SCD under DSM-5, according to the APA.
Under DSM-5, there was a statistically significant decrease in AD diagnosis of 22 percent, compared with the fourth edition of the manual, the meta-analysis found. There was also a statistically significant decrease of 70 percent in diagnosis of PDD-NOS. While diagnosis of Asperger's also declined under DSM-5, the reduction was not statistically significant. In addition, the study found that some individuals who no longer met the criteria for an ASD diagnosis under DSM-5 would also fail to meet the criteria for SCD.
“We are potentially going to lose diagnosis and treatment for some of the most vulnerable kids who have developmental delays,” says Kulage. “In many instances, children require a diagnosis of ASD to receive medical benefits, educational support and social services.”
Approximately 1 in 88 children in the U.S. have ASD, according to the Centers for Disease Control and Prevention. People with ASD tend to have difficulties with communication, misread nonverbal interactions, and have difficulty making friends. They may also be heavily reliant on routines, extremely sensitive to changes in their environment, and intensely focused on interests not appropriate to the social context they are in. Symptoms fall on a continuum, with variation in severity, and early diagnosis and access to treatment have been proven to result in better outcomes.
The paper is titled: “How Will DSM-5 Affect Autism Diagnosis? A Systematic Literature Review and Meta-analysis” and it appeared in the February 2014 issue of the Journal of Autism and Developmental Disorders. Other contributors are: from Columbia Nursing, Arlene Smaldone, PhD, CPNP, associate professor and assistant dean, scholarship and research, and Elizabeth Cohn, PhD, RN, assistant professor and Robert Wood Johnson Foundation Nurse Faculty Scholar. Kulage completed the research while enrolled in a master's degree program at Joseph P. Mailman School of Public Health.
The authors declare no financial or other conflicts of interest.
Columbia University School of Nursing is part of the Columbia University Medical Center, which also includes the College of Physicians & Surgeons, the Mailman School of Public Health, and the College of Dental Medicine. With close to 100 full-time faculty and 600 students, the School of Nursing is dedicated to educating the next generation of nurse leaders in education, research, and clinical care. The School has pioneered advanced practice nursing curricula and continues to define the role of nursing and nursing research through its PhD program which prepares nurse scientists, and its Doctor of Nursing Practice (DNP), the first clinical practice doctorate in the nation. Among the clinical practice areas shaped by the School's research are the reduction of infectious disease and the use of health care informatics to improve health and health care. For more information, please visit: http://www.nursing.columbia.edu.
Media Contact
All latest news from the category: Health and Medicine
This subject area encompasses research and studies in the field of human medicine.
Among the wide-ranging list of topics covered here are anesthesiology, anatomy, surgery, human genetics, hygiene and environmental medicine, internal medicine, neurology, pharmacology, physiology, urology and dental medicine.
Newest articles
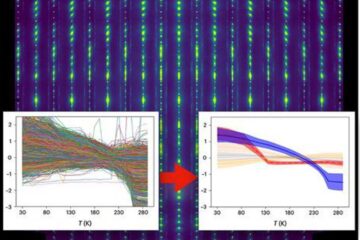
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















