Pooled data towards cervical cancer cure

Half of all the 60,000 new cases of cervical cancer diagnosed in Europe this year will prove to be incurable and result in the patient’s death, and a similar percentage of the hundreds of thousands of women diagnosed worldwide will also die.
To make any impact on these statistics, medical researchers will need access to huge amounts of data on cervical cancer victims, the sort of data collected and analysed in what medical professionals call Association Studies.
Thanks to the work of the 2008 Nobel Prize-winning scientist, Harald zur Hausen, we know that cervical cancer is caused by the human papilloma virus (HPV). But not every woman infected with the virus develops the disease, while some of those who do develop it respond to treatment, and others do not. There is also the complication that there are many different variants of HPV, and not all of them cause cancer.
To try and understand these discrepancies in different patients, and what the root causes are, it is necessary to examine as much information as possible about as many patients as possible to try and identify common factors. Association Studies do this by studying clinical data from hospital tests, lifestyle data such as eating, smoking and sexual habits and genetic data. They also compare the data with that from healthy patients not infected by the virus.
Forging links between hospitals
Until now, these tests have generally been undertaken at individual clinics and medical centres where researchers only had access to data concerning tens or perhaps hundreds of patients. The EU-funded ASSIST project was set up to forge technological links between leading medical centres specialising in the diagnosis and treatment of cervical cancer, to allow them to share data and thus create a much larger data repository.
Says project coordinator Professor Pericles Mitkas of the Centre for Research and Technology – Hellas, Informatics and Telematics Institute, Thessaloniki: “What we are trying to do is to allow medical researchers working in specialist hospitals and medical centres to use each others’ data, and combine the data into a bigger pool to work with.”
While this may sound logical and easy, in practise it is not. “The problem is, each hospital uses different formats, different rules for storing data, even for exactly the same tests. Even within hospitals, each doctor might have his or her own way of doing things,” says Mitkas.
The challenge is primarily an IT one, but it requires doctors from various disciplines – researchers, microbiologists and geneticists at the different centres – to agree to adopt common practices for the system to work.
Agreeing on a common terminology
“Perhaps the greatest achievement of the project to date has been to get medical doctors, molecular biologists and computer scientists sitting around a table and talking to each other, and finally understanding each other’s technical language,” says Mitkas.
There are three hospitals involved in the initial stage of the project, from Greece, Germany and Belgium. Mitkas says it was also an achievement to get the doctors from these institutions to agree to “common terminology, common ground, and a common view on how to represent data and access it.”
With these agreements in place, the team developed a prototype software platform which ensures researchers get data reported back to them in a similar format and in the exact way in which it was requested. “We do this by semantic representation, which means we assign an interpretation to each value to help the computer understand what each value refers to,” Mitkas explains.
“We also facilitate interpretation of subjective values like ‘high risk’ and ‘low risk’, ‘serious cases’ and ‘non-serious cases’, and use inferencing techniques which are based on a set of medical rules provided by doctors to tell the computer which results are more valid than others. Biopsy results, for example, are more conclusive than Pap test results and may point to a pre-cancer stage that a Pap test did not reveal.”
Greatly expanded data pool
Working with the three hospitals, the ASSIST prototype platform now allows researchers access to thousands of patients’ records at the gynaecology and obstetrics departments of the three hospitals, including the results of annual tests on all women, not just those infected.
“We add extra functionality as we go along, but at least the doctors now have something to work with and evaluate,” says Mitkas.
The project recently hosted a conference where the platform was introduced to some of the leading cervical cancer specialists from around Europe, and they were so impressed that several of them have agreed to add their data to the ASSIST pool.
In the future, the work done on this project can be applied to other types of cancer, with just some adjustments being needed to the software to cope with different data sets, Mitkas suggests. And there is no reason why the platform cannot be used with other types of disease such as cardiovascular, he says.
“Further down the line, understanding the path to the disease and the factors that affect it will help individual doctors diagnose it earlier, prevent it by giving directions to their patients, and developing drugs or procedures that will cure the disease. But ASSIST is primarily a tool for medical researchers, and the results of their research will benefit all women,” Mitkas concludes.
Media Contact
All latest news from the category: Medical Engineering
The development of medical equipment, products and technical procedures is characterized by high research and development costs in a variety of fields related to the study of human medicine.
innovations-report provides informative and stimulating reports and articles on topics ranging from imaging processes, cell and tissue techniques, optical techniques, implants, orthopedic aids, clinical and medical office equipment, dialysis systems and x-ray/radiation monitoring devices to endoscopy, ultrasound, surgical techniques, and dental materials.
Newest articles

Silicon Carbide Innovation Alliance to drive industrial-scale semiconductor work
Known for its ability to withstand extreme environments and high voltages, silicon carbide (SiC) is a semiconducting material made up of silicon and carbon atoms arranged into crystals that is…

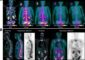
New SPECT/CT technique shows impressive biomarker identification
…offers increased access for prostate cancer patients. A novel SPECT/CT acquisition method can accurately detect radiopharmaceutical biodistribution in a convenient manner for prostate cancer patients, opening the door for more…

How 3D printers can give robots a soft touch
Soft skin coverings and touch sensors have emerged as a promising feature for robots that are both safer and more intuitive for human interaction, but they are expensive and difficult…