Simple Steps Prevent Life-Threatening Bloodstream Infections in Children

Yearlong research led by Marlene Miller, M.D. Ms.C., of the Johns Hopkins Children’s Center with colleagues from other hospitals saw a 43 percent drop in the rate of bloodstream infections from catheters in 29 pediatric intensive care units (PICUs) that focused on careful placement and basic daily cleaning of the devices.
Results are to be published in the February issue of the journal Pediatrics.
Each year, 250,000 central line infections occur in the United States, researchers estimate, and up to one-fourth of patients die from them. Between 10 and 20 percent of children who get such infections die from them, researchers believe, and each infection carries a cost of $50, 000.
“If every single pediatric intensive care unit applies this approach rigorously and systematically, I’d be surprised if it didn’t translate into hundreds of lives and millions of dollars saved,” says Miller. Miller serves as vice president for quality transformation at the National Association of Children’s Hospitals and Related Institutions (NACHRI), which spearheaded the initiative.
A central venous catheter, or central line, is a tube inserted into a major blood vessel in the neck, chest or groin to serve as a temporary portal for injected medications and fluids, or blood sampling in patients who need them frequently. Because central lines also provide quick access in emergencies, children in the PICU often have them for weeks or longer. But if inserted incorrectly and, more importantly, mishandled after that, the central line can become a contaminated gateway for bacteria to enter directly into the patient’s bloodstream.
Therefore, investigators say, simple precautions like regularly changing the dressing covering the central line, changing the tubes and caps attached to it, cleaning the line before and after use, and rigorous hand washing before handling the line are essential to keeping bacteria away.
The new research also showed that while proper placement and daily care were both important in reducing catheter-related bloodstream infections, proper daily maintenance played the greatest role in preventing infections in children.
“Children, for example, may require more frequent blood draws through their catheter than adult patients so their central lines are handled more frequently on a day-to-day basis, which makes routine care for the device that much more critical in children than in adults,” Miller says.
The research further showed that medical staff compliance with day-to-day handling of central lines increased from 65 percent to 82 percent during the study period, suggesting that continuing education of medical staff and reminders to follow catheter protocol should be a mainstay in every PICU.
The research, launched as part of a nationwide effort to minimize preventable complications and deaths from this commonly used intravenous device, continues with more than 40 PICUs joining the initiative over the last two years. The effort continues today with more than 60 PICUs and is focused on further improving daily practices for central line handling.
Co-investigators include Michael Griswold, Ph.D., and Gayane Yenokyan, M.D. M.P.H. , of the Johns Hopkins Bloomberg School of Public Health; Mitchell Harris II, Ph.D., NACHRI; Charles Huskins, M.D., Mayo Clinic; Michele Moss, M.D., Arkansas Children’s Hospital; Tom Rice, M.D., Children’s Hospital of Wisconsin; Debra Ridling, R.N. , M.S., C.C.R.N., Children’s Hospital and Regional Medical Center, Seattle; Deborah Campbell, R.N., C. C.C.R.N., Kasair Children’s Hospital; Peter Margolis, M.D. Ph.D., Center for Child Health Quality; Richard Brilli, M.D., Nationwide Children’s Hospital.
Founded in 1912 as the children's hospital of the Johns Hopkins Medical Institutions, the Johns Hopkins Children's Center offers one of the most comprehensive pediatric medical programs in the country, treating more than 90,000 children each year. Hopkins Children’s is consistently ranked among the top children's hospitals in the nation. Hopkins Children’s is Maryland's largest children’s hospital and the only state-designated Trauma Service and Burn Unit for pediatric patients. It has recognized Centers of Excellence in dozens of pediatric subspecialties, including allergy, cardiology, cystic fibrosis, gastroenterology, nephrology, neurology, neurosurgery, oncology, pulmonary, and transplant. For more information, please visit www.hopkinschildrens.org
Media Contact
All latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
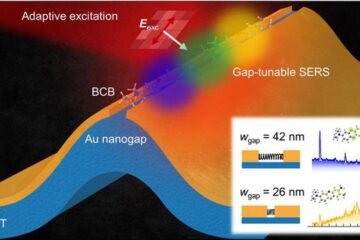
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















