Scientists discover genetic switch that can prevent peripheral vascular disease in mice

Working to develop a new treatment for peripheral vascular disease from left to right are UTHealth researchers Vikas Yadav, Ph.D., Sabina Lorca and Vihang Narkar, Ph.D. Credit: The University of Texas Health Science Center at Houston (UTHealth)
At The University of Texas Health Science Center at Houston (UTHealth) Medical School, scientists tested a non-surgical preventative treatment in a mouse model of the disease and it was associated with increased blood circulation. Their proof-of-concept study appears in the journal Cell Reports.
Unlike previous studies in which other investigators used individual stimulatory factors to grow blood vessels, Vihang Narkar, Ph.D., senior author and assistant professor in the Department of Integrative Biology and Pharmacology at the UTHealth Medical School, identified and turned off a genetic switch that stifles blood vessel development.
“We discovered an inhibitory switch that degrades blood vessels,” said Narkar, whose laboratory is in the UTHealth Center for Metabolic and Degenerative Diseases at The Brown Foundation Institute of Molecular Medicine for the Prevention of Human Diseases. “We were able to genetically turn it off to prevent peripheral vascular disease in a preclinical study.”
Added Narkar, “Our next step will be to test this targeted treatment in models of other conditions that dramatically decrease circulation like diabetes and atherosclerosis.”
Narkar said using individual growth factors to stimulate blood vessel growth often leads to the formation of leaky and non-functional blood vessels. “By turning off a genetic switch that acts as a roadblock for blood vessel growth, we were able to trigger and accelerate the natural process of blood vessel regeneration that involves a battery of growth factors,” he said.
The switch is called peroxisome proliferator-activated receptor gamma co-activator 1 beta (PGC1beta) and could be a key to future treatments for additional conditions like cardiac myopathies, cancer and retinopathy.
Narkar's UTHealth co-authors are Vikas Yadav, Ph.D. (lead author), Antonios Matsakas, Ph.D., and Sabina Lorca. Narkar is on the faculty of The University of Texas Graduate School of Biomedical Sciences at Houston.
The study titled “PGC1beta activates anti-angiogenic program to repress neo-angiogenesis in muscle ischemia” received support from the American Heart Association (AHA#11SDG7600213), American Diabetes Association (ADA#1-13-BS-127) and Muscular Dystrophy Association (MDA#174408).
Media Contact
All latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles
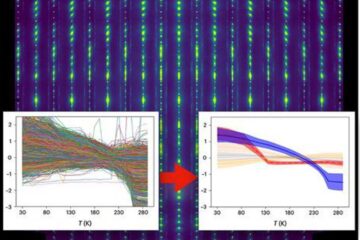
Machine learning algorithm reveals long-theorized glass phase in crystal
Scientists have found evidence of an elusive, glassy phase of matter that emerges when a crystal’s perfect internal pattern is disrupted. X-ray technology and machine learning converge to shed light…

Mapping plant functional diversity from space
HKU ecologists revolutionize ecosystem monitoring with novel field-satellite integration. An international team of researchers, led by Professor Jin WU from the School of Biological Sciences at The University of Hong…

Inverters with constant full load capability
…enable an increase in the performance of electric drives. Overheating components significantly limit the performance of drivetrains in electric vehicles. Inverters in particular are subject to a high thermal load,…





















