One Path – Two Effects: Immune System uses DNA Repair Mechanism to Boost Defence

How does the immune system manage to keep pace with this diversity? For the first time scientists from the GSF – Research Centre for Environment and Health and the Max-Planck-Institute for Biochemistry in Martinsried could show that a molecular mechanism which is normally needed to repair damaged DNA pieces makes cells of the immune system particularly variable, so that they can react flexibly to a wide range of pathogens.
Certain defence cells of the immune system, the B-cells, are responsible for the production of specific antibodies. “These cells are the only body cells which can change their DNA by hypermutation, so that they form antibodies which are specifically tailored to the respective pathogen,” Prof. Jean-Marie Buerstedde, the Director of the GSF Institute of Molecular Radiation Biology, explains. Hypermutation is understood to be a considerably elevated mutation rate. The genes coding for specific antibodies mutate one million times more frequently than the genes of other cells.
It has been known for a long time that hypermutation is triggered by the enzyme AID. “AID is the master gene for hypermutation,” Buerstedde explains. It is B-cell-specific and causes a particular base of the DNA to be converted into another. This “wrong” base is then cut out of the DNA, which eventually creates a base gap. Buerstedde and his colleagues have now been able to prove that the following steps of the hypermutation make use of a mechanism which is also responsible for repairing damaged DNA. If the B-cell DNA is incomplete, the protein PCNA will be linked with another protein, ubiquitin – this mechanism activates certain emergency enzymes which mend the base gap as repair enzymes. PCNA ubiquitination also comes into action in normal body cells when the DNA is damaged: in this case, however, this mechanism ensures that DNA damage is repaired in a quick-fix procedure during the replication of the DNA. “Thus, PCNA ubiquitination is necessary both for DNA repair and for hypermutation,” Buerstedde explains.
PCNA ubiquitination in B-cells results in high mutation rates, since the emergency enzymes activated by this mechanism are highly likely to build not the original, but a different base into the DNA – the consequence being a point mutation. Several of these point mutations raise the affinity of the antibodies to a particular antigen and thus make the antibodies produced more effective. By antigen binding those B-cells are selected, which best bind the antigen and can, therefore, combat it most intensively. The remaining cells will die.
Thus, the immune system has tailored the path of PCNA ubiquitination for the use in B-cells for itself in such a way that high mutation rates occur in certain parts of the antibody genes. “On the one hand this is positive, because variable antibodies result. On the other hand, there is also the risk that uncontrolled mutations on wrong genes will contribute to the development of B-cell cancer. Therefore, the exploration of this path is of medical relevance,” Buerstedde emphasizes, “but for a geneticist it is just as exciting to realize that vertebrates adopted a path for the antigen-specific immune response, which has existed since primeval times”.
Media Contact
More Information:
http://www.gsf.de/neu/Aktuelles/Presse/2006/buerstedde_en.phpAll latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
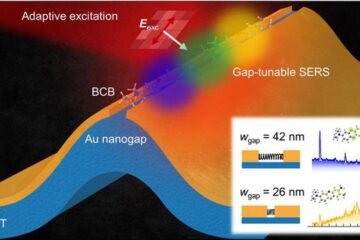
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















