New gene marker may identify need for intense AML therapy

Researchers here have discovered a new marker that might identify a serious form of acute myeloid leukemia (AML) in people who lack the signs that normally alert doctors that the patient needs intense therapy.
The study was led by researchers with The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute. It focused on AML patients whose cancer cells show none of the chromosome alterations that help doctors determine the probable prognosis and the best potential treatment for many people with acute leukemia.
Specifically, the study examined the activity of a gene known as ETS-Related Gene (ERG) in AML cells from these patients.
The findings, published online in the Journal of Clinical Oncology, suggest that when AML cells show high ERG activity, it signals an aggressive form of cancer that requires intense therapy, such as a stem-cell transplant from a matched donor.
Importantly, the study also showed that effects of ERG activity on disease relapse and long-term survival are influenced by the activity levels of other genes.
Last, the study suggests that ERG plays an important role in AML development and could provide a new target for future AML therapy.
The findings come from a Cancer and Leukemia Group B (CALGB) study led by Clara D. Bloomfield, professor of internal medicine, the William G. Pace III Professor in Cancer Research, OSU Cancer Scholar and senior adviser to the OSU Cancer Program.
“This is another of only a few predictive molecular markers for adults with AML who have normal cytogenetics,” says Bloomfield, who led the research that identified the first molecular marker for AML in this group of patients. Normal cytogenetics refers to cells with normal-looking chromosomes.
“If confirmed, our findings should improve survival in these patients and spare those who now receive more intense therapy but don’t need it.”
About 55 percent of AML patients have cancer cells showing chromosome alterations at the time of diagnosis. Doctors rely on these alterations to help determine the best therapy for these patients and the likelihood of remission and cure.
But the cancer cells in about 45 percent of AML patients have normal-looking chromosomes, giving doctors few clues for choosing therapy. Overall about 40 percent of these patients are alive after five years following intensive therapy.
“This means that 60 percent of patients relapse,” Bloomfield says, “and that probably happens because those who relapse have unidentified gene mutations and molecular changes that affect survival and their response to treatment.
“Some examples of these mutations and molecular changes have already been identified. ERG is probably another, and I have no doubt that more will be found.”
The present study tested whether activity levels of ERG are related to remission and survival rates in AML patients with normal cytogenetics.
(Levels of gene activity, or more correctly, gene expression, refers to whether a gene is highly, moderately or not engaged in the production of a protein. Gene-expression levels are determined by measuring the number of RNA copies of the gene that are present in cells. A high number of RNA copies indicates a high level of gene activity; a low number indicates low gene activity.)
The study examined samples of cancer cells from 84 AML patients under age 60 years who had normal cytogenetics. The samples were analyzed for the activity levels of ERG and other genes known to influence treatment response in these patients.
The 84 samples were then divided into four groups according to ERG activity. The group with high ERG activity was compared with the other three groups combined in terms of the patients’ relapse and survival rates.
In general, the group with high ERG did extremely poorly compared with the other groups when consider by itself and in combination with other genes.
When the researchers looked at the likelihood of relapse and the influence of high ERG by itself, they found that 81 percent of high ERG patients relapsed after five years versus 33 percent of patients in the other groups.
However, when the risk of relapse was examined in combination with a second gene known as MLL PTD, patients with high ERG were four times more likely to relapse than the patients with low ERG..
When the researchers considered survival and the influence of ERG alone, they found that the group with high ERG lived an average of 1.2 years following treatment, while the other three groups had not yet reached their average survival when the study ended.
When the researchers then examined the impact of ERG in combination with other factors on survival, they found that the patients who did best had low ERG and low activity of a gene known as BAALC. Seventy percent of these patients were alive after five years.
“This study is important because we have found another gene (ERG) that seems to have a major influence in this large subset of AML patients,” Bloomfield says, “and we’ve identified other genes that alter ERG’s effects on relapse and survival.”
Overall, the evidence strongly indicates that ERG may play a key role in leukemia development. Therefore, a drug that is designed to reduce ERG activity, perhaps in combination with chemotherapy or other targeted therapy, “might prevent these patients from relapsing,” Bloomfield says, “and that would be quite a success.”
Other OSU researchers involved in this study were Guido Marcucci, Claudia D. Baldus, Amy S. Ruppert, Krzysztof Mrozek, Susan P. Whitman, Colin G. Edwards, Danilo Perrotti, Michael A. Caligiuri and Albert de la Chapelle.
Funding from the National Cancer Institute and The Coleman Leukemia Research Foundation supported this research.
Media Contact
More Information:
http://www.osumc.eduAll latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
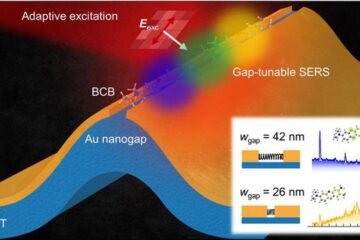
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















