Pinpointing a tell-tale mark of liver cancer

Persistent hepatitis C virus (HCV) infection can lead to chronic hepatitis C and then progress to fatal liver diseases including liver cirrhosis and liver cancer, the third most common cause of cancer-related deaths.
Worldwide, more than 170 million people are infected with HCV, and the virus accounts for 30–70% of liver cancer cases. The recent identification of a genetic variant associated with increased susceptibility to hepatitis C virus-induced liver cancer could have major implications for global healthcare, as it may lead to tests that predict liver cancer susceptibility.
Michiaki Kubo of the RIKEN Center for Genomic Medicine and colleagues from RIKEN and The University of Tokyo discovered the variant by analyzing the entire genomes of 721 Japanese individuals with HCV-induced liver cancer and comparing them with those of 2,890 HCV-negative controls1. This allowed them to identify variants potentially associated HCV-induced liver cancer . They confirmed the association of one variant by replicating the study in another 673 liver cancer patients and 2,596 controls.
This variant was located within a region on chromosome 6, which contains many genes that are critical for immune system function. It lies between the genes encoding MICA, a membrane protein that activates the anti-tumor effects of white blood cells, and the HLA-B gene, which encodes a peptide that enables the immune system to distinguish between the body’s own proteins and those produced by invading microbes.
The researchers checked the variant in another 1,730 individuals with chronic hepatitis C who had not developed liver cirrhosis or liver cancer, and revealed that it was significantly associated with progression from chronic hepatitis C to liver cancer, but not with susceptibility to chronic hepatitis C.
Finally, Kubo and colleagues examined MICA protein levels in patients with chronic hepatitis C and HCV-induced liver cirrhosis, and found that the level of MICA in blood samples was elevated during early stages of the disease compared to healthy controls. They also found that the identified variant was correlated with low MICA levels in patients with chronic hepatitis C.
These findings suggest that individuals carrying the genetic variant would express low levels of MICA. This in turn would lead to reduced response by white blood cells to cells infected with viruses, increasing the likelihood of progression from chronic hepatitis C to liver cancer.
“Our results suggest that low serum MICA levels are a marker for higher susceptibility to progression of liver cancer in the patients with chronic hepatitis C,” says Kubo.
The corresponding author for this highlight is based at the Laboratory for Genotyping Development, RIKEN Center for Genomics Medicine
Reference:
Kumar, V., Kato, N., Urabe, Y., Takahashi, A., Muroyama, R., Hosono, N., Otsuka, M., Tateishi, R., Omata, M., Nakagawa, H. et al. Genome-wide association study identifies a susceptibility locus for HCV-induced hepatocellular carcinoma. Nature Genetics 43, 455–458 (2011).
Media Contact
All latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
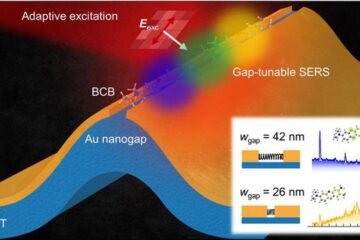
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















