Fruitfly study: Epilepsy drug target implications for sleep disruption in brain disorders
This image shows the proximity of GABA-producing neurons (green) and glia (purple) in the fly brain. Credit: Amita Sehgal, Ph.D., Perelman School of Medicine, University of Pennsylvania
The findings, published online in Molecular Psychiatry, were led by Amita Sehgal, PhD, head of the Chronobiology Program at the University of Pennsylvania's Perelman School of Medicine.
The findings shed light on mechanisms that may be shared between sleep disruption and some neurological disorders. A better understanding of this connection could enable treatments that target both types of symptoms and perhaps provide better therapeutic efficacy.
“Epilepsy is essentially an increase-in-firing disorder of the brain and maybe a decrease in activity of the neurotransmitter GABA, too,” says Sehgal, who is also a professor of Neuroscience and an investigator with the Howard Hughes Medical Institute (HHMI).
“This connects our work to drugs that inhibit GABA transaminase. Changes in GABA transaminase activity are implicated in epilepsy and some other psychiatric disorders, which may account for some of the associated sleep problems.”
The team looked at the proteomics of the sss mutant brain – a large-scale study of the structure and function of related proteins — and found that GABA transaminase is increased in the sss brain compared to controls. This enzyme breaks down GABA, so GABA is decreased in the sss brain. Because GABA promotes sleep, there is a decrease in sleep in the sss mutant fly, as the name implies.
The relationship between the SSS protein and GABA is not fully understood. The SSS protein controls neural activity, and its absence results in increased neural firing, which likely uses up a lot of energy, says Sehgal.
GABA transaminase works in the mitochondria, the energy-production organelle in the glial cells of the brain, which provide fuel for neurons. The large energy demand created by the increased neural firing in sss brains probably alters mitochondrial metabolism, including GABA transaminase function in glia.
In the sss mutant fly, there is a stream of connections that leads to its signature loss of sleep: The sss mutant has increased neuron firing caused by downregulation of a potassium channel protein called Shaker. Recently, the Sehgal lab showed that SSS also affects activity of acetylcholine receptors.
Both of these actions may directly cause an inability to sleep. In addition, increased energy demands on glia, which increase GABA transaminase and decrease GABA, may further contribute to sleep loss. On the other hand, if GABA is increased, then sleep is increased, as in flies that lack GABA transaminase.
Coauthors are Wen-Feng Chen, Sarah Maguire, Mallory Sowcik, Wenyu Luo, all from Penn and Kyunghee Koh from Thomas Jefferson University. The study was funded by HHMI.
Penn Medicine is one of the world's leading academic medical centers, dedicated to the related missions of medical education, biomedical research, and excellence in patient care. Penn Medicine consists of the Raymond and Ruth Perelman School of Medicine at the University of Pennsylvania (founded in 1765 as the nation's first medical school) and the University of Pennsylvania Health System, which together form a $4.3 billion enterprise.
The Perelman School of Medicine has been ranked among the top five medical schools in the United States for the past 17 years, according to U.S. News & World Report's survey of research-oriented medical schools. The School is consistently among the nation's top recipients of funding from the National Institutes of Health, with $392 million awarded in the 2013 fiscal year.
The University of Pennsylvania Health System's patient care facilities include: The Hospital of the University of Pennsylvania — recognized as one of the nation's top “Honor Roll” hospitals by U.S. News & World Report; Penn Presbyterian Medical Center; Chester County Hospital; Penn Wissahickon Hospice; and Pennsylvania Hospital — the nation's first hospital, founded in 1751. Additional affiliated inpatient care facilities and services throughout the Philadelphia region include Chestnut Hill Hospital and Good Shepherd Penn Partners, a partnership between Good Shepherd Rehabilitation Network and Penn Medicine.
Penn Medicine is committed to improving lives and health through a variety of community-based programs and activities. In fiscal year 2013, Penn Medicine provided $814 million to benefit our community.
Media Contact
All latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

“Nanostitches” enable lighter and tougher composite materials
In research that may lead to next-generation airplanes and spacecraft, MIT engineers used carbon nanotubes to prevent cracking in multilayered composites. To save on fuel and reduce aircraft emissions, engineers…

Trash to treasure
Researchers turn metal waste into catalyst for hydrogen. Scientists have found a way to transform metal waste into a highly efficient catalyst to make hydrogen from water, a discovery that…
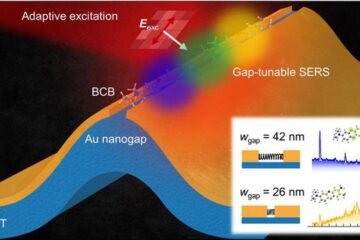
Real-time detection of infectious disease viruses
… by searching for molecular fingerprinting. A research team consisting of Professor Kyoung-Duck Park and Taeyoung Moon and Huitae Joo, PhD candidates, from the Department of Physics at Pohang University…





















