Developmental protein plays role in spread of cancer
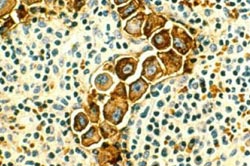
This image shows metastasized human breast cancer cells (magnified 400 times, stained brown) in lymph nodes. Credit: Image courtesy of National Cancer Institute<br>
Metastasis is responsible for 90 percent of cancer-related deaths. More than 575,000 Americans die of cancer each year, the second leading cause of death in the United States after cardiovascular disease.
The scientists, led by principal investigator Thomas Kipps, MD, PhD, Evelyn and Edwin Tasch Chair in Cancer Research at UC San Diego, discovered an association between the protein, called Receptor-tyrosine-kinase-like Orphan Receptor 1 or ROR1, and the epithelial-mesenchymal transition (EMT), a process that occurs during embryogenesis when cells migrate and then grow into new organs during early development.
In research published in 2012, Kipps and colleagues reported for the first time that ROR1 is expressed during embryogenesis and by many different types of cancers, but not by normal post-partum tissues. They also discovered that silencing the protein impaired the growth and survival of human breast cancer cells.
In their latest work, the scientists found that high-level expression of ROR1 in breast cancer cells correlates to higher rates of relapse and metastasis in patients with breast adenocarcinoma, a type of cancer that originates in glandular tissue. Conversely, silencing expression of ROR1 reverses EMT and inhibits the metastatic spread of breast cancer cells in animal models. Moreover, the researchers found that treatment with a monoclonal antibody targeting ROR1 also could inhibit the growth and spread of highly metastatic tumors that express ROR1.
“We might think of ROR1 as an oncogene,” said study co-author Bing Cui, PhD, a postdoctoral fellow in Kipps' lab. “This means ROR1 has some tumor initiation functions. However, ROR1 also appears to allow transformed cells to invade other tissues and to promote tumor expansion in both the primary tumor site and in distant organs.”
Because ROR1 is expressed only in cancer cells, Kipps' team says it presents a singular, selective target for anti-cancer therapies that would leave normal cells unaffected. It's not yet clear how the monoclonal antibody approach, tested thus far only in culture and animal models, impacts primary tumors, said Cui, but it does offer promise for inhibiting the spread of cancer. The researchers are developing a humanized monoclonal antibody for potential clinical studies in patients with cancers that express ROR1.
Co-authors are Suping Zhang, Liguang Chen, Jianqiang Yu, George F. Widhopf II, Jessie F. Fecteau and Laura Z. Rassenti, all of UC San Diego Moores Cancer Center and the Department of Medicine, UCSD.
Funding for this research came, in part, from the National Institutes of Health (grant PO1-CA081534), the California Institute of Regenerative Medicine and the Blood Cancer Research Fund, UC San Diego Foundation.
Media Contact
More Information:
http://www.ucsd.eduAll latest news from the category: Life Sciences and Chemistry
Articles and reports from the Life Sciences and chemistry area deal with applied and basic research into modern biology, chemistry and human medicine.
Valuable information can be found on a range of life sciences fields including bacteriology, biochemistry, bionics, bioinformatics, biophysics, biotechnology, genetics, geobotany, human biology, marine biology, microbiology, molecular biology, cellular biology, zoology, bioinorganic chemistry, microchemistry and environmental chemistry.
Newest articles

Combatting disruptive ‘noise’ in quantum communication
In a significant milestone for quantum communication technology, an experiment has demonstrated how networks can be leveraged to combat disruptive ‘noise’ in quantum communications. The international effort led by researchers…

Stretchable quantum dot display
Intrinsically stretchable quantum dot-based light-emitting diodes achieved record-breaking performance. A team of South Korean scientists led by Professor KIM Dae-Hyeong of the Center for Nanoparticle Research within the Institute for…

Internet can achieve quantum speed with light saved as sound
Researchers at the University of Copenhagen’s Niels Bohr Institute have developed a new way to create quantum memory: A small drum can store data sent with light in its sonic…





















